Drug Information
General Information of This Drug
| Drug ID | DRG00039 | |||||
|---|---|---|---|---|---|---|
| Drug Name | Morphine-6-glucuronide | |||||
| Target(s) | Mu-type opioid receptor (OPRM1) | Target Info | ||||
| Structure |
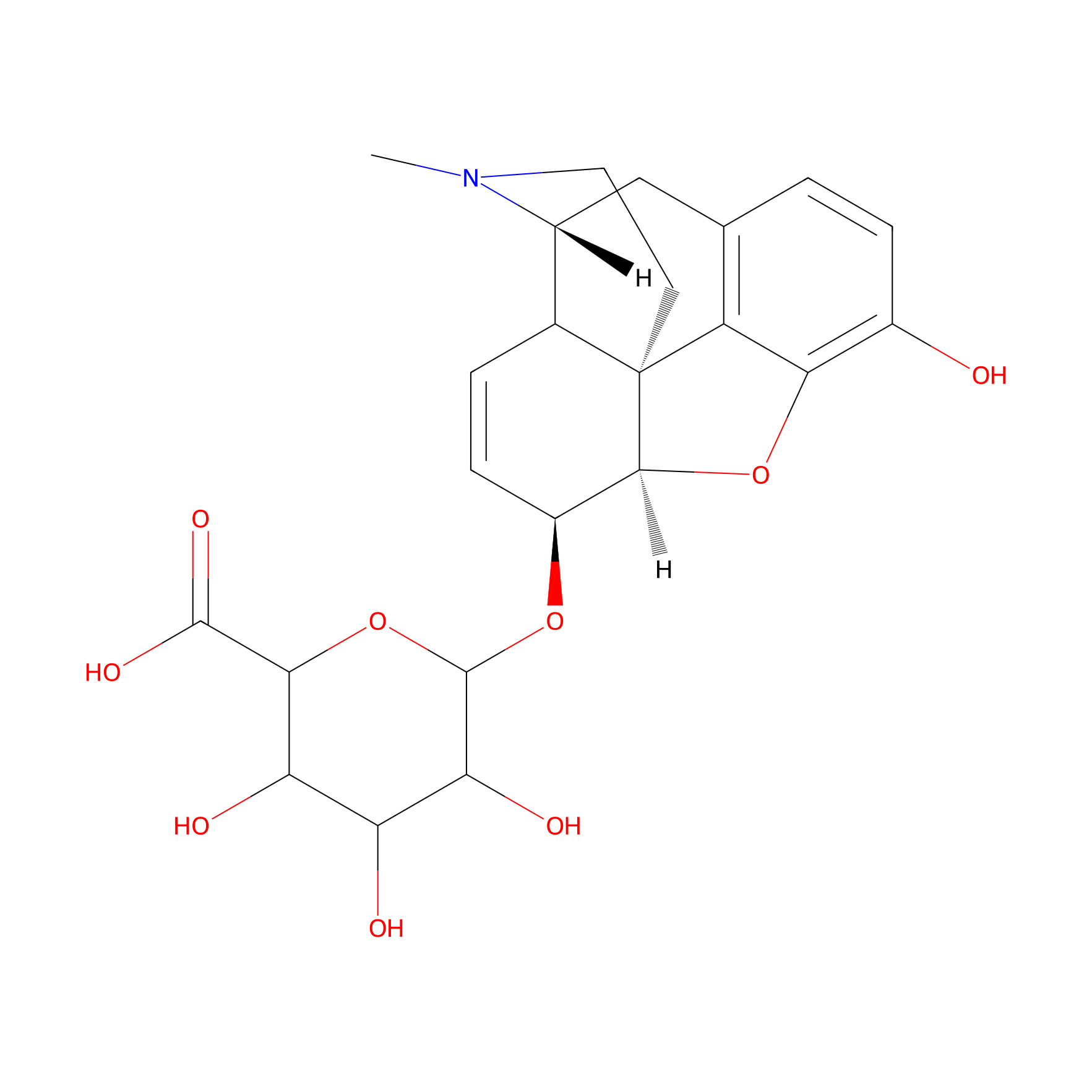
|
|||||
| Formula |
C23H27NO9
|
|||||
| #Ro5 Violations (Lipinski): 1 | Molecular Weight (mw) | 461.5 | ||||
| Lipid-water partition coefficient (xlogp) | -2.9 | |||||
| Hydrogen Bond Donor Count (hbonddonor) | 5 | |||||
| Hydrogen Bond Acceptor Count (hbondacc) | 10 | |||||
| Rotatable Bond Count (rotbonds) | 3 | |||||
| PubChem CID | ||||||
| Canonical smiles |
CN1CCC23C4C1CC5=C2C(=C(C=C5)O)OC3C(C=C4)OC6C(C(C(C(O6)C(=O)O)O)O)O
|
|||||
| InChI |
InChI=1S/C23H27NO9/c1-24-7-6-23-10-3-5-13(31-22-17(28)15(26)16(27)19(33-22)21(29)30)20(23)32-18-12(25)4-2-9(14(18)23)8-11(10)24/h2-5,10-11,13,15-17,19-20,22,25-28H,6-8H2,1H3,(H,29,30)/t10?,11-,13+,15?,16?,17?,19?,20+,22?,23+/m1/s1
|
|||||
| InChIKey |
GNJCUHZOSOYIEC-AMYPAFSWSA-N
|
|||||
| IUPAC Name |
6-[[(4R,7S,7aR,12bS)-9-hydroxy-3-methyl-2,4,4a,7,7a,13-hexahydro-1H-4,12-methanobenzofuro[3,2-e]isoquinolin-7-yl]oxy]-3,4,5-trihydroxyoxane-2-carboxylic acid
|
|||||
The activity data of This Drug
| Standard Type | Value | Administration times | Administration dosage | Vivo model | Ref. | |
|---|---|---|---|---|---|---|
| Maximal antinociceptive effect | 40% | Intravenous administration 30min | 3 mg/kg | Male CD1 mice. | [1] | |
| Maximal antinociceptive effect | 68% | Subcutaneous administration 60min | 4.5 mg/kg | Rat model. | [1] | |
| Maximal antinociceptive effect | 87% | Intravenous administration 45min | 4.5 mg/kg | Rat model. | [1] | |
Each Peptide-drug Conjugate Related to This Drug
Full Information of The Activity Data of The PDC(s) Related to This Drug
An2-M6G [Preclinical]
Obtained from the Model Organism Data
| Experiment 1 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Severe pain | ||||
| Efficacy Data | Maximal antinociceptive effect | 34.90% | |||
| Evaluation Method | Rat tail-flick test assay | ||||
| Administration Time | Intravenous administration 60 min | ||||
| Administration Dosage | 4 mg/kg | ||||
| MOA of PDC |
Given the high analgesic potency of M6G, without induction of the M3G metabolite that antagonizes the analgesic effect of morphine, M6G could be a promising drug to treat moderate to severe pain. The major issue of systemic use of M6G is its poor BBB permeability. In this study, we proposed to increase the BBB penetration of M6G and morphine by conjugation to the shuttle angiopep-2 peptide (An2). Morphine and M6G were first conjugated to An2, a 19-mer peptide that crosses the BBB by low-density lipoprotein receptor-related protein 1 (LRP1) receptor-mediated transcytosis.
Click to Show/Hide
|
||||
| Description |
Indeed, at an equimolar dose of 3 mg/kg of morphine (i.e., 12 mg/kg), An2-M6G produced a latency to tail withdrawal reaching the cutoff (i.e., 10 seconds) after 30 minutes, an effect lasting at least 3 hours. The %MPE calculated at 60 minutes after the intravenous injection of An2-M6G at 4, 8, and 12 mg/kg (equivalent to 1, 2, and 3 mg/kg of morphine and to 1.5, 3, and 4.5 mg/kg of M6G) was 34.9%, 66.2%, and 100%, respectively.
Click to Show/Hide
|
||||
| In Vivo Model | Rat model. | ||||
| Experiment 2 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Severe pain | ||||
| Efficacy Data | Maximal antinociceptive effect | 66.20% | |||
| Evaluation Method | Rat tail-flick test assay | ||||
| Administration Time | Intravenous administration 60 min | ||||
| Administration Dosage | 8 mg/kg | ||||
| MOA of PDC |
Given the high analgesic potency of M6G, without induction of the M3G metabolite that antagonizes the analgesic effect of morphine, M6G could be a promising drug to treat moderate to severe pain. The major issue of systemic use of M6G is its poor BBB permeability. In this study, we proposed to increase the BBB penetration of M6G and morphine by conjugation to the shuttle angiopep-2 peptide (An2). Morphine and M6G were first conjugated to An2, a 19-mer peptide that crosses the BBB by low-density lipoprotein receptor-related protein 1 (LRP1) receptor-mediated transcytosis.
Click to Show/Hide
|
||||
| Description |
Indeed, at an equimolar dose of 3 mg/kg of morphine (i.e., 12 mg/kg), An2-M6G produced a latency to tail withdrawal reaching the cutoff (i.e., 10 seconds) after 30 minutes, an effect lasting at least 3 hours. The %MPE calculated at 60 minutes after the intravenous injection of An2-M6G at 4, 8, and 12 mg/kg (equivalent to 1, 2, and 3 mg/kg of morphine and to 1.5, 3, and 4.5 mg/kg of M6G) was 34.9%, 66.2%, and 100%, respectively.
Click to Show/Hide
|
||||
| In Vivo Model | Rat model. | ||||
| Experiment 3 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Severe pain | ||||
| Efficacy Data | Maximal antinociceptive effect | 74% | |||
| Evaluation Method | Rat tail-flick test assay | ||||
| Administration Time | Subcutaneous administration 200 min | ||||
| Administration Dosage | 12 mg/kg | ||||
| MOA of PDC |
Given the high analgesic potency of M6G, without induction of the M3G metabolite that antagonizes the analgesic effect of morphine, M6G could be a promising drug to treat moderate to severe pain. The major issue of systemic use of M6G is its poor BBB permeability. In this study, we proposed to increase the BBB penetration of M6G and morphine by conjugation to the shuttle angiopep-2 peptide (An2). Morphine and M6G were first conjugated to An2, a 19-mer peptide that crosses the BBB by low-density lipoprotein receptor-related protein 1 (LRP1) receptor-mediated transcytosis.
Click to Show/Hide
|
||||
| Description |
We also measured the analgesic effect of An2-morphine and An2-M6G after subcutaneous injections. Despite similar MPE at the peak effect, subcutaneous injection of 20 mg/kg An2-morphine (equivalent to 5.5 mg/kg of morphine) produced an analgesic effect that was more prolonged over the time than what was observed with an equimolar dose of morphine.
|
||||
| In Vivo Model | Rat model. | ||||
| Experiment 4 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Severe pain | ||||
| Efficacy Data | Maximal antinociceptive effect | 100% | |||
| Evaluation Method | Rat tail-flick test assay | ||||
| Administration Time | Intravenous administration 60 min | ||||
| Administration Dosage | 12 mg/kg | ||||
| MOA of PDC |
Given the high analgesic potency of M6G, without induction of the M3G metabolite that antagonizes the analgesic effect of morphine, M6G could be a promising drug to treat moderate to severe pain. The major issue of systemic use of M6G is its poor BBB permeability. In this study, we proposed to increase the BBB penetration of M6G and morphine by conjugation to the shuttle angiopep-2 peptide (An2). Morphine and M6G were first conjugated to An2, a 19-mer peptide that crosses the BBB by low-density lipoprotein receptor-related protein 1 (LRP1) receptor-mediated transcytosis.
Click to Show/Hide
|
||||
| Description |
Indeed, at an equimolar dose of 3 mg/kg of morphine (i.e., 12 mg/kg), An2-M6G produced a latency to tail withdrawal reaching the cutoff (i.e., 10 seconds) after 30 minutes, an effect lasting at least 3 hours. The %MPE calculated at 60 minutes after the intravenous injection of An2-M6G at 4, 8, and 12 mg/kg (equivalent to 1, 2, and 3 mg/kg of morphine and to 1.5, 3, and 4.5 mg/kg of M6G) was 34.9%, 66.2%, and 100%, respectively.
Click to Show/Hide
|
||||
| In Vivo Model | Rat model. | ||||
| Experiment 5 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Severe pain | ||||
| Efficacy Data | Maximal antinociceptive effect | 100% | |||
| Evaluation Method | Hot-plate test assay | ||||
| Administration Time | Intravenous administration 30 min | ||||
| Administration Dosage | 6 mg/kg | ||||
| MOA of PDC |
Given the high analgesic potency of M6G, without induction of the M3G metabolite that antagonizes the analgesic effect of morphine, M6G could be a promising drug to treat moderate to severe pain. The major issue of systemic use of M6G is its poor BBB permeability. In this study, we proposed to increase the BBB penetration of M6G and morphine by conjugation to the shuttle angiopep-2 peptide (An2). Morphine and M6G were first conjugated to An2, a 19-mer peptide that crosses the BBB by low-density lipoprotein receptor-related protein 1 (LRP1) receptor-mediated transcytosis.
Click to Show/Hide
|
||||
| Description |
Similar results were also obtained in the hot-plate test using male CD1 mice. Over a 2-hour period, both morphine and An2-morphine caused similar increases in hot-plate latencies. Likewise, mice receiving An2-M6G (6 mg/kg i.v.) also exhibited a sustained and superior analgesic effect compared with equimolar doses of either morphine or M6G.
|
||||
| In Vivo Model | Male CD1 mice. | ||||
References
