Drug Information
General Information of This Drug
| Drug ID | DRG00406 | |||||
|---|---|---|---|---|---|---|
| Drug Name | Monastrol | |||||
| Synonyms |
monastrol; 329689-23-8; 254753-54-3; DL-Monastrol; ETHYL 4-(3-HYDROXYPHENYL)-6-METHYL-2-THIOXO-1,2,3,4-TETRAHYDROPYRIMIDINE-5-CARBOXYLATE; 4-(3-Hydroxyphenyl)-6-methyl-2-thioxo-1,2,3,4-tetrahydro-4H-pyrimidin-5-carboxylic Acid Ethyl Ester; ethyl 4-(3-hydroxyphenyl)-6-methyl-2-sulfanylidene-3,4-dihydro-1H-pyrimidine-5-carboxylate; CHEBI:75382; ethyl 4-(3-hydroxyphenyl)-6-methyl-2-sulfanylidene-1,2,3,4-tetrahydropyrimidine-5-carboxylate; (+/-)-Monastrol; 5-Pyrimidinecarboxylic acid,1,2,3,4-tetrahydro-4-(3-hydroxyphenyl)-6-methyl-2-thioxo-, ethyl ester; SR-01000357662; Monastrol?; ()-Monastrol; MFCD00813077; ( inverted exclamation markA)-Monastrol; (A+/-)-Monastrol; Probes1_000001; Probes1_000042; Probes1_000312; Probes2_000257; Probes2_000376; Lopac0_000821; Oprea1_487786; BSPBio_001273; CBDivE_015834; KBioGR_000613; KBioSS_000613; MLS006011746; C18H23NO3S; F3284-6466; SCHEMBL3168349; BCBcMAP01_000162; KBio2_000613; KBio2_003181; KBio2_005749; KBio3_001085; KBio3_001086; DTXSID10388124; CHEBI:143544; LOBCDGHHHHGHFA-UHFFFAOYSA-N; BDBM175356; Bio1_000459; Bio1_000948; Bio1_001437; Bio2_000467; Bio2_000947; DTXSID501317756; GLXC-04725; HMS1362O15; HMS1792O15; HMS1990O15; HMS3267N03; HMS3403O15; HMS3412E20; HMS3676E20; BCP06757; BCP19385; EX-A1988; EX-A4169; GR-322; HB2551; MFCD06762956; NSC716782; NSC829695; s8439; STK386781; ZINC00297106; Monastrol, >=98% (HPLC), solid; AKOS000295413; AKOS002264887; AKOS016068396; AKOS016315550; CCG-267397; CS-6183; HY-101071A; NSC-716782; NSC-829695; IDI1_002222; SMP1_000197; UPCMLD0ENAT5762435:001; NCGC00025103-01; NCGC00025103-02; NCGC00025103-03; NCGC00025103-04; AC-33010; AS-74678; NCI60_040353; SMR004703468; DB-048305; D84039; M 8515; EN300-1266062; A902103; J-016007; Q6898425; SR-01000357662-1; SR-01000357662-2; BRD-A78377521-001-02-2; BRD-A78377521-001-03-0; BRD-A78377521-001-05-5; Z57061994; 5-[[4-[(1-Methylcyclohexyl)methoxy] phenyl]methyl]-2,4-thiazolidinedione; Ethyl 4-(3-hydroxyphenyl)-6-methyl-2-thioxo-1,2,3,4-tetrahydro-4H-pyrimidin-5-carboxylate; ethyl 4-(3-hydroxyphenyl)-6-methyl-2-thioxo-3,4-dihydro-1H-pyrimidine-5-carboxylate; ethyl 6-(3-hydroxyphenyl)-2-mercapto-4-methyl-1,6-dihydropyrimidine-5-carboxylate; ethyl 6-methyl-4-(3-hydroxyphenyl)-2-thioxo-1,2,3,4-tetrahydropyrimidine-5-carboxylate; rac-ethyl 4-(3-hydroxyphenyl)-6-methyl-2-thioxo-1,2,3,4-tetrahydropyrimidine-5-carboxylate; 6-Methyl-4-(3-hydroxyphenyl)-2-thioxo-1,2,3,4-tetrahydropyrimidine-5-carboxylic acid ethyl ester; Ethyl 4-(3-hydroxyphenyl)-6-methyl-2-thioxo-1,2,3,4-tetrahydropyrimidine-5-carboxylate (11)
Click to Show/Hide
|
|||||
| Target(s) | Kinesin-like protein KIF11 (KIF11) | Target Info | ||||
| Structure |
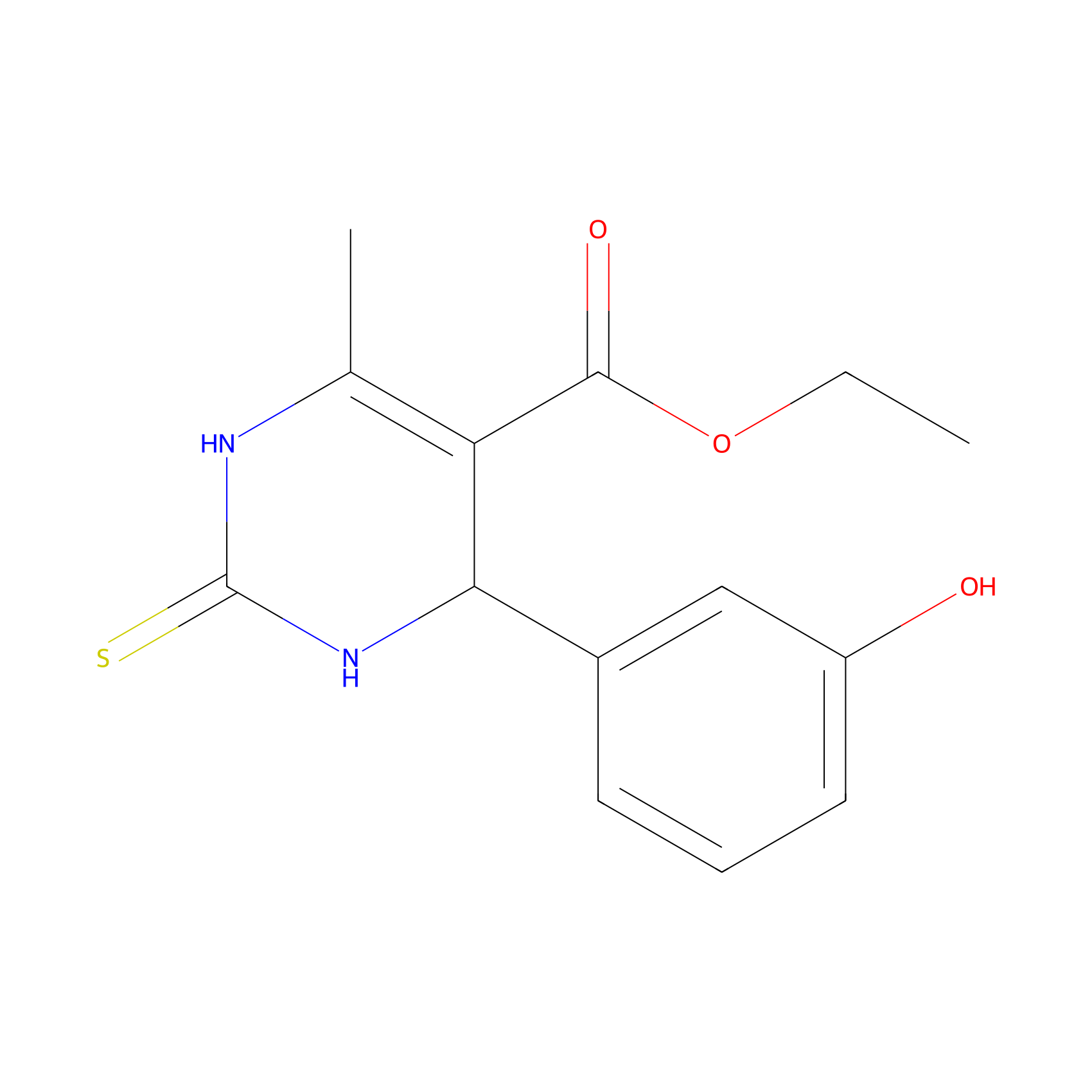
|
|||||
| Formula |
C14H16N2O3S
|
|||||
| #Ro5 Violations (Lipinski): 0 | Molecular Weight (mw) | 292.36 | ||||
| Lipid-water partition coefficient (xlogp) | 1.6 | |||||
| Hydrogen Bond Donor Count (hbonddonor) | 3 | |||||
| Hydrogen Bond Acceptor Count (hbondacc) | 4 | |||||
| Rotatable Bond Count (rotbonds) | 4 | |||||
| PubChem CID | ||||||
| Canonical smiles |
CCOC(=O)C1=C(NC(=S)NC1C2=CC(=CC=C2)O)C
|
|||||
| InChI |
InChI=1S/C14H16N2O3S/c1-3-19-13(18)11-8(2)15-14(20)16-12(11)9-5-4-6-10(17)7-9/h4-7,12,17H,3H2,1-2H3,(H2,15,16,20)
|
|||||
| InChIKey |
LOBCDGHHHHGHFA-UHFFFAOYSA-N
|
|||||
| IUPAC Name |
ethyl 4-(3-hydroxyphenyl)-6-methyl-2-sulfanylidene-3,4-dihydro-1H-pyrimidine-5-carboxylate
|
|||||
The activity data of This Drug
| Standard Type | Value | Disease Model | Cell line | Cell line ID | Ref. | |
|---|---|---|---|---|---|---|
| Half Maximal Effective Concentration (EC50) | 1.2 uM | Colon carcinoma | HCT 116 cell | CVCL_0291 | [1] | |
| Half Maximal Growth Inhibition (GI50) | 31.6 uM | T acute lymphoblastic leukemia | CCRF-CEM cell | CVCL_0207 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 31.6 uM | T acute lymphoblastic leukemia | MOLT-4 cell | CVCL_0013 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 31.6 uM | Normal | COLO205 cell | CVCL_F402 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 31.6 uM | Non-small cell lung carcinoma | NCI-H522 cell | CVCL_1567 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 31.6 uM | Melanoma | SK-MEL-2 cell | CVCL_0069 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 31.6 uM | Leukemia | SR cell | CVCL_1711 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 31.6 uM | Glioblastoma | SF-295 cell | CVCL_1690 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 31.6 uM | Colon adenocarcinoma | KM12 cell | CVCL_1331 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 31.6 uM | Chronic myeloid leukemia | K562 cell | CVCL_0004 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 39.8 uM | Renal cell carcinoma | SN12C cell | CVCL_1705 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 39.8 uM | Minimally invasive lung adenocarcinoma | NCI-H322M cell | CVCL_1557 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 39.8 uM | Glioblastoma | SNB-75 cell | CVCL_1706 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 39.8 uM | Cutaneous melanoma | SK-MEL-5 cell | CVCL_0527 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 39.8 uM | Colon adenocarcinoma | HCC 2998 cell | CVCL_1266 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 39.8 uM | Colon adenocarcinoma | SW620 cell | CVCL_0547 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 39.8 uM | Colon adenocarcinoma | HCT 15 cell | CVCL_0292 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 50.1 uM | Pleural epithelioid mesothelioma | NCI-H226 cell | CVCL_1544 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 50.1 uM | Ovarian serous adenocarcinoma | OVCAR-3 cell | CVCL_0465 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 50.1 uM | Ovarian endometrioid adenocarcinoma | IGROV-1 cell | CVCL_1304 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 50.1 uM | Gliosarcoma | SF539 cell | CVCL_1691 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 63.1 uM | Ovarian serous cystadenocarcinoma | SK-OV-3 cell | CVCL_0532 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 63.1 uM | Ovarian adenocarcinoma | OVCAR-4 cell | CVCL_1627 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 63.1 uM | Non-small cell lung carcinoma | EKVX cell | CVCL_1195 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 63.1 uM | Melanoma | UACC-257 cell | CVCL_1779 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 63.1 uM | Melanoma | Malme-3M cell | CVCL_1438 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 63.1 uM | Lung adenocarcinoma | NCI-H23 cell | CVCL_1547 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 79.4 uM | Renal adenocarcinoma | ACHN cell | CVCL_1067 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 79.4 uM | Ovarian serous adenocarcinoma | OVCAR-5 cell | CVCL_1628 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 79.4 uM | Melanoma | LOX IMVI cell | CVCL_1381 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 79.4 uM | Cutaneous melanoma | SK-MEL-28 cell | CVCL_0526 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 79.4 uM | Colon cancer | HT29 cell | CVCL_A8EZ | [2] | |
| Half Maximal Growth Inhibition (GI50) | 79.4 uM | Astrocytoma | SNB-19 cell | CVCL_0535 | [2] | |
| Half Maximal Growth Inhibition (GI50) | 100 uM | Renal carcinoma | UO-31 cell | CVCL_1911 | [2] | |
| Half Maximal Inhibitory Concentration (IC50) | 45 ug/mL | Invasive breast carcinoma | MCF-7 cell | CVCL_0031 | [3] | |
| Half Maximal Inhibitory Concentration (IC50) | >10 uM | Lung adenocarcinoma | A-549 cell | CVCL_0023 | [4] | |
| Half Maximal Inhibitory Concentration (IC50) | >10 uM | Gastric adenocarcinoma | AGS cell | CVCL_0139 | [4] | |
| Half Maximal Inhibitory Concentration (IC50) | >100 uM | Lung adenocarcinoma | A-549 cell | CVCL_0023 | [5] | |
Each Peptide-drug Conjugate Related to This Drug
Full Information of The Activity Data of The PDC(s) Related to This Drug
NT4-MON ether [Investigative]
Revealed Based on the Cell Line Data
| Experiment 1 Reporting the Activity Data of This PDC | [6] | ||||
| Indication | Solid tumor | ||||
| Efficacy Data | Cell viability | 0.00% | |||
| Administration Time | 6 days | ||||
| Administration Dosage | 0.03 mM | ||||
| MOA of PDC |
We have been studying protease-resistant branched peptides as tumor targeting agents by using tetra-branched peptides (NT4) containing the human regulatory peptide neurotensin (NT) sequence. Neurotensin receptors are overexpressed in several human malignancies, such as colon, pancreatic, prostate and small-cell lung cancer. We have been using NT4 conjugated to different functional units for tumor imaging and therapy, and found that NT4 conjugated to methotrexate produced 60% reduction of tumor growth in xenografted mice. Results obtained with NT4 indicated that branched peptides are promising novel multifunctional targeting molecules, which might allow cancer detection and therapy by means of the same molecule, with no modification in target binding, but rather a simple exchange of functional units. Since cancer cells are very different from one another in terms of drug sensibility, not only in different tumors but in different patients and stages of the disease, this approach prefigures the synthesis of a number of constructs conjugated with differently acting chemotherapeutics. The type of linkage between effector unit (drug/imaging agent etc.) and peptide is obviously crucial for this type of approach. The choice must be driven by two issues: 1) The nature of the drug functional groups available for coupling with the peptide; and 2) the mechanism-of-action of the drug. When a prodrug acts without being released from the carrier unit, a strong linker is preferred. However, if a drug has to be released in order to interact with the intracellular target, the linker must be cleavable. In latter, the linker has to be chosen properly-not too labile or leakage will occur during drug distribution, but not too robust or the pharmacological action will be impaired.
Click to Show/Hide
|
||||
| Description |
This clearly indicated that the chemotherapeutic moiety was released into the cell medium and the drug was internalized into the cells, probably by membrane diffusion. This became evident when observing the behavior of the unrelated conjugated peptides.
|
||||
| In Vitro Model | Prostate carcinoma | PC-3 cell | CVCL_0035 | ||
| Experiment 2 Reporting the Activity Data of This PDC | [6] | ||||
| Indication | Solid tumor | ||||
| Efficacy Data | Cell viability | 5.00% | |||
| Administration Time | 6 days | ||||
| Administration Dosage | 0.03 mM | ||||
| MOA of PDC |
We have been studying protease-resistant branched peptides as tumor targeting agents by using tetra-branched peptides (NT4) containing the human regulatory peptide neurotensin (NT) sequence. Neurotensin receptors are overexpressed in several human malignancies, such as colon, pancreatic, prostate and small-cell lung cancer. We have been using NT4 conjugated to different functional units for tumor imaging and therapy, and found that NT4 conjugated to methotrexate produced 60% reduction of tumor growth in xenografted mice. Results obtained with NT4 indicated that branched peptides are promising novel multifunctional targeting molecules, which might allow cancer detection and therapy by means of the same molecule, with no modification in target binding, but rather a simple exchange of functional units. Since cancer cells are very different from one another in terms of drug sensibility, not only in different tumors but in different patients and stages of the disease, this approach prefigures the synthesis of a number of constructs conjugated with differently acting chemotherapeutics. The type of linkage between effector unit (drug/imaging agent etc.) and peptide is obviously crucial for this type of approach. The choice must be driven by two issues: 1) The nature of the drug functional groups available for coupling with the peptide; and 2) the mechanism-of-action of the drug. When a prodrug acts without being released from the carrier unit, a strong linker is preferred. However, if a drug has to be released in order to interact with the intracellular target, the linker must be cleavable. In latter, the linker has to be chosen properly-not too labile or leakage will occur during drug distribution, but not too robust or the pharmacological action will be impaired.
Click to Show/Hide
|
||||
| Description |
This clearly indicated that the chemotherapeutic moiety was released into the cell medium and the drug was internalized into the cells, probably by membrane diffusion. This became evident when observing the behavior of the unrelated conjugated peptides.
|
||||
| In Vitro Model | Colon adenocarcinoma | HT-29 cell | CVCL_0320 | ||
| Experiment 3 Reporting the Activity Data of This PDC | [6] | ||||
| Indication | Solid tumor | ||||
| Efficacy Data | Cell viability | 50.00% | |||
| Administration Time | 6 days | ||||
| Administration Dosage | 0.03 mM | ||||
| MOA of PDC |
We have been studying protease-resistant branched peptides as tumor targeting agents by using tetra-branched peptides (NT4) containing the human regulatory peptide neurotensin (NT) sequence. Neurotensin receptors are overexpressed in several human malignancies, such as colon, pancreatic, prostate and small-cell lung cancer. We have been using NT4 conjugated to different functional units for tumor imaging and therapy, and found that NT4 conjugated to methotrexate produced 60% reduction of tumor growth in xenografted mice. Results obtained with NT4 indicated that branched peptides are promising novel multifunctional targeting molecules, which might allow cancer detection and therapy by means of the same molecule, with no modification in target binding, but rather a simple exchange of functional units. Since cancer cells are very different from one another in terms of drug sensibility, not only in different tumors but in different patients and stages of the disease, this approach prefigures the synthesis of a number of constructs conjugated with differently acting chemotherapeutics. The type of linkage between effector unit (drug/imaging agent etc.) and peptide is obviously crucial for this type of approach. The choice must be driven by two issues: 1) The nature of the drug functional groups available for coupling with the peptide; and 2) the mechanism-of-action of the drug. When a prodrug acts without being released from the carrier unit, a strong linker is preferred. However, if a drug has to be released in order to interact with the intracellular target, the linker must be cleavable. In latter, the linker has to be chosen properly-not too labile or leakage will occur during drug distribution, but not too robust or the pharmacological action will be impaired.
Click to Show/Hide
|
||||
| Description |
This clearly indicated that the chemotherapeutic moiety was released into the cell medium and the drug was internalized into the cells, probably by membrane diffusion. This became evident when observing the behavior of the unrelated conjugated peptides.
|
||||
| In Vitro Model | Pancreatic ductal adenocarcinoma | PANC-1 cell | CVCL_0480 | ||
References
