Peptide Information
General Information of This Peptide
| Peptide ID |
PEP00108
|
|||||
|---|---|---|---|---|---|---|
| Peptide Name |
3-Tyr-Octreotide
|
|||||
| Structure |
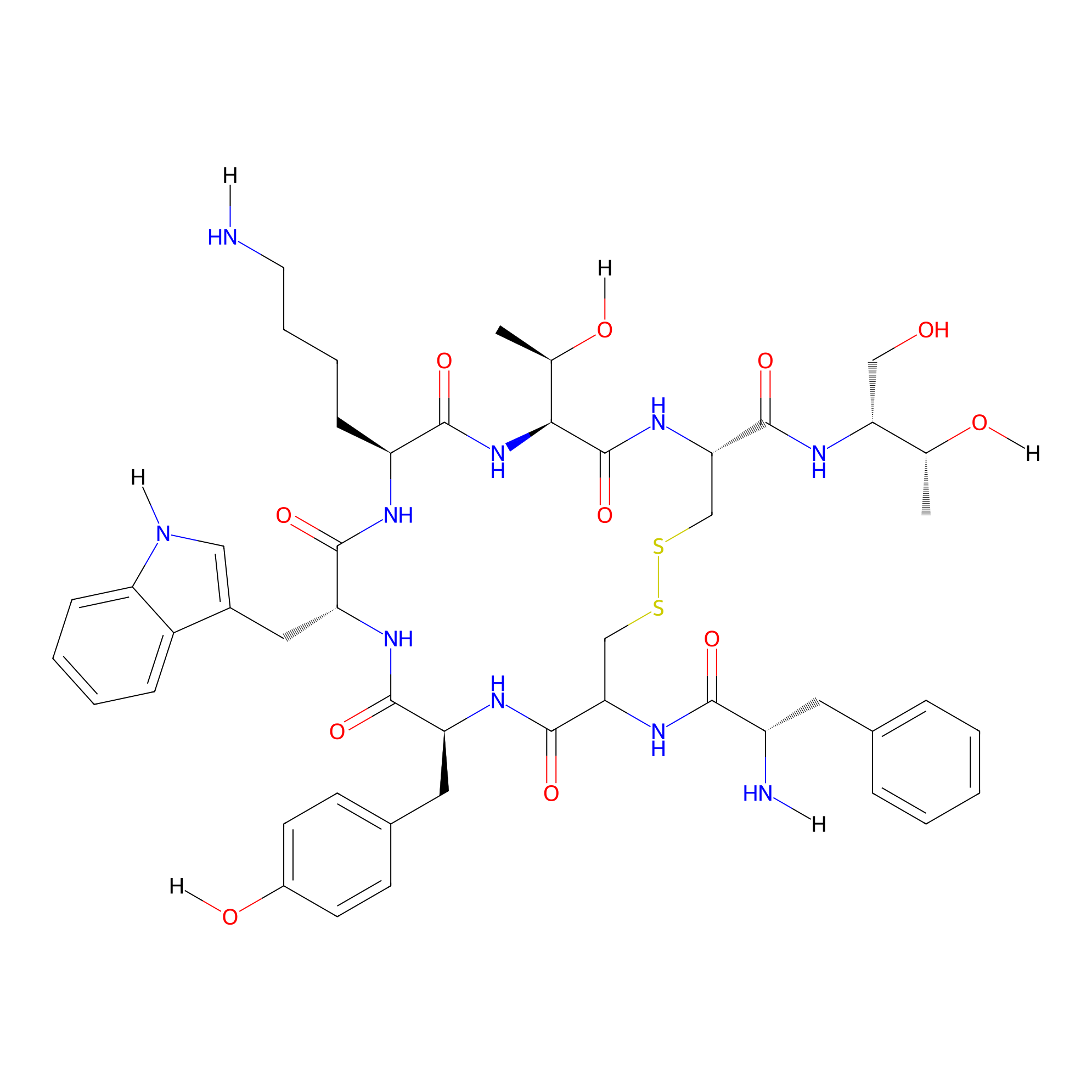
|
|||||
| Sequence |
NH2-FCYWKTCT
|
|||||
| Peptide Type |
Cyclic
|
|||||
| Receptor Name |
Somatostatin receptor type 1 (SSTR1)
|
Receptor Info | ||||
| PDC Transmembrane Types | Cell targeting peptides (CTPs) | |||||
| Formula |
C49H66N10O11S2
|
|||||
| Isosmiles |
[H]NCCCC[C@@H]1NC(=O)[C@@H](Cc2cn([H])c3ccccc23)NC(=O)[C@H](Cc2ccc(O[H])cc2)NC(=O)C(NC(=O)[C@H](Cc2ccccc2)N[H])CSSC[C@@H](C(=O)N[C@]([H])(CO)[C@@H](C)O[H])NC(=O)[C@]([H])([C@@H](C)O[H])NC1=O
|
|||||
| InChI |
InChI=1S/C49H66N10O11S2/c1-27(61)39(24-60)56-48(69)41-26-72-71-25-40(57-43(64)34(51)20-29-10-4-3-5-11-29)47(68)54-37(21-30-15-17-32(63)18-16-30)45(66)55-38(22-31-23-52-35-13-7-6-12-33(31)35)46(67)53-36(14-8-9-19-50)44(65)59-42(28(2)62)49(70)58-41/h3-7,10-13,15-18,23,27-28,34,36-42,52,60-63H,8-9,14,19-22,24-26,50-51H2,1-2H3,(H,53,67)(H,54,68)(H,55,66)(H,56,69)(H,57,64)(H,58,70)(H,59,65)/t27-,28-,34+,36+,37+,38-,39-,40?,41+,42+/m1/s1
|
|||||
| InChIKey |
LHCIROHUTQLZCZ-FFFGXVRSSA-N
|
|||||
| Pharmaceutical Properties |
Molecule Weight
|
1035.26
|
Polar area
|
352.45
|
||
|
Complexity
|
1034.435395
|
xlogp Value
|
-1.0998
|
|||
|
Heavy Count
|
72
|
Rot Bonds
|
22
|
|||
|
Hbond acc
|
15
|
Hbond Donor
|
14
|
|||
Each Peptide-drug Conjugate Related to This Peptide
Full Information of The Activity Data of The PDC(s) Related to This Peptide
67Ga-MMC(TMZ)-TOC [Investigative]
Discovered Using Cell Line-derived Xenograft Model
| Experiment 1 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Pancreatic serotonin-producing neuroendocrine tumor | ||||
| Efficacy Data | Surviving fraction |
80%
|
|||
| Administration Time | 5 days | ||||
| Administration Dosage | 2 μmol/L | ||||
| Evaluation Method | Colony-forming assay | ||||
| MOA of PDC |
In this study, we hypothesized that the clinically utilized radiopharmaceutical 68Ga-DOTA-TOC could be converted to a radiolabeled peptide-drug conjugate (PDC) for selective delivery of TMZ to SSTR2-positive tumor cells. We used the intrinsic radiolabeling utility of the PDC to characterize receptor-binding properties, pharmacokinetics (PK), and tissue biodistribution in cells and animal studies. Receptor-targeted DNA-damaging properties and cytotoxic effects of the PDC were examined in different cell lines, and the effects of accumulated doses on MGMT content were evaluated in MGMT-positive cells.
Click to Show/Hide
|
||||
| Description |
TMZ is an alkylating agent that causes cell death through DNA-damaging mechanisms.?To determine whether MMC(TMZ)-TOC induces the same cytotoxic effects through a receptor-dependent process, we first studied its DNA-damaging properties in IMR-32 cells that endogenously express SSTR2. We performed an alkaline comet assay to evaluate the ability of our drug conjugate to produce single- and double-stranded DNA breaks. As shown in?Figure 3A,B, the targeted agent-induced DNA breaks that were similar to free TMZ, resulting in migrating DNA fragments (comet tail) from the nucleoid (comet head). The damaging effects of MMC(TMZ)-TOC were significantly reduced (P?< 0.0001) when cells were preincubated with blocking doses of the high-affinity SSTR2 antagonist JR11, indicating receptor-dependent cytotoxicity. Next, we used a colony formation assay to assess the long-term survival and reproductive capability of the cells after treatment with the PDC. We treated BON1 (receptor-negative) and BON1-SSTR2 (receptor-positive) cells with 2 mu;mol/L MMC(TMZ)-TOC or 10 mu;mol/L TMZ for 5 consecutive days, seeded the cells at a low-density number, and allowed them to grow and form colonies for 14 days. The clonogenic survival data showed that MMC(TMZ)-TOC produced cytotoxic effects in the receptor-positive BON1-SSTR2 cells (P?< 0.01) similar to clinically relevant doses of TMZ. Conversely, no cytotoxicity was observed in receptor-negative BON1 cells following treatment with the drug conjugate, further illustrating the receptor-dependent effects of the PDC.
Click to Show/Hide
|
||||
| In Vivo Model | Dually implanted HCT116-WT/SSTR2 mice xenograft models. | ||||
| In Vitro Model | Pancreatic serotonin-producing neuroendocrine tumor | BON-1 cell | CVCL_3985 | ||
| Experiment 2 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Pancreatic serotonin-producing neuroendocrine tumor | ||||
| Efficacy Data | Surviving fraction |
100%
|
|||
| Administration Time | 5 days | ||||
| Administration Dosage | 2 μmol/L | ||||
| Evaluation Method | Colony-forming assay | ||||
| MOA of PDC |
In this study, we hypothesized that the clinically utilized radiopharmaceutical 68Ga-DOTA-TOC could be converted to a radiolabeled peptide-drug conjugate (PDC) for selective delivery of TMZ to SSTR2-positive tumor cells. We used the intrinsic radiolabeling utility of the PDC to characterize receptor-binding properties, pharmacokinetics (PK), and tissue biodistribution in cells and animal studies. Receptor-targeted DNA-damaging properties and cytotoxic effects of the PDC were examined in different cell lines, and the effects of accumulated doses on MGMT content were evaluated in MGMT-positive cells.
Click to Show/Hide
|
||||
| Description |
TMZ is an alkylating agent that causes cell death through DNA-damaging mechanisms.?To determine whether MMC(TMZ)-TOC induces the same cytotoxic effects through a receptor-dependent process, we first studied its DNA-damaging properties in IMR-32 cells that endogenously express SSTR2. We performed an alkaline comet assay to evaluate the ability of our drug conjugate to produce single- and double-stranded DNA breaks. As shown in?Figure 3A,B, the targeted agent-induced DNA breaks that were similar to free TMZ, resulting in migrating DNA fragments (comet tail) from the nucleoid (comet head). The damaging effects of MMC(TMZ)-TOC were significantly reduced (P?< 0.0001) when cells were preincubated with blocking doses of the high-affinity SSTR2 antagonist JR11, indicating receptor-dependent cytotoxicity. Next, we used a colony formation assay to assess the long-term survival and reproductive capability of the cells after treatment with the PDC. We treated BON1 (receptor-negative) and BON1-SSTR2 (receptor-positive) cells with 2 mu;mol/L MMC(TMZ)-TOC or 10 mu;mol/L TMZ for 5 consecutive days, seeded the cells at a low-density number, and allowed them to grow and form colonies for 14 days. The clonogenic survival data showed that MMC(TMZ)-TOC produced cytotoxic effects in the receptor-positive BON1-SSTR2 cells (P?< 0.01) similar to clinically relevant doses of TMZ. Conversely, no cytotoxicity was observed in receptor-negative BON1 cells following treatment with the drug conjugate, further illustrating the receptor-dependent effects of the PDC.
Click to Show/Hide
|
||||
| In Vivo Model | Dually implanted HCT116-WT/SSTR2 mice xenograft models. | ||||
| In Vitro Model | Pancreatic serotonin-producing neuroendocrine tumor | BON-1 cell | CVCL_3985 | ||
MMC(TMZ)-TOC [Investigative]
Revealed Based on the Cell Line Data
| Experiment 1 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Neuroendocrine tumour | ||||
| Efficacy Data | Survival rate |
80%
|
|||
| Administration Time | 4-6 h/day for 5 consecutive days | ||||
| Administration Dosage | 2 µmol/L | ||||
| Evaluation Method | Colony-forming assay | ||||
| MOA of PDC |
In this study, we hypothesized that the clinically utilized radiopharmaceutical 68Ga-DOTA-TOC could be converted to a radiolabeled peptide-drug conjugate (PDC) for selective delivery of TMZ to SSTR2-positive tumor cells. We used the intrinsic radiolabeling utility of the PDC to characterize receptor-binding properties, pharmacokinetics (PK), and tissue biodistribution in cells and animal studies. Receptor-targeted DNA-damaging properties and cytotoxic effects of the PDC were examined in different cell lines, and the effects of accumulated doses on MGMT content were evaluated in MGMT-positive cells.
Click to Show/Hide
|
||||
| Description |
TMZ is an alkylating agent that causes cell death through DNA-damaging mechanisms. To determine whether MMC(TMZ)-TOC induces the same cytotoxic effects through a receptor-dependent process, we first studied its DNA-damaging properties in IMR-32 cells that endogenously express SSTR2. We performed an alkaline comet assay to evaluate the ability of our drug conjugate to produce single- and double-stranded DNA breaks. As shown in Figure 3A,B, the targeted agent-induced DNA breaks that were similar to free TMZ, resulting in migrating DNA fragments (comet tail) from the nucleoid (comet head). The damaging effects of MMC(TMZ)-TOC were significantly reduced (P < 0.0001) when cells were preincubated with blocking doses of the high-affinity SSTR2 antagonist JR11, indicating receptor-dependent cytotoxicity. Next, we used a colony formation assay to assess the long-term survival and reproductive capability of the cells after treatment with the PDC. We treated BON1 (receptor-negative) and BON1-SSTR2 (receptor-positive) cells with 2 umol/L MMC(TMZ)-TOC or 10 umol/L TMZ for 5 consecutive days, seeded the cells at a low-density number, and allowed them to grow and form colonies for 14 days. The clonogenic survival data showed that MMC(TMZ)-TOC produced cytotoxic effects in the receptor-positive BON1-SSTR2 cells (P < 0.01) similar to clinically relevant doses of TMZ. Conversely, no cytotoxicity was observed in receptor-negative BON1 cells following treatment with the drug conjugate, further illustrating the receptor-dependent effects of the PDC.
Click to Show/Hide
|
||||
| In Vitro Model | SSR2 positive neuroendocrine tumour | BON1-SSTR2 cell | CVCL_3985 | ||
| Experiment 2 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Neuroendocrine tumour | ||||
| Efficacy Data | Survival rate |
100%
|
|||
| Administration Time | 4-6 h/day for 5 consecutive days | ||||
| Administration Dosage | 2 µmol/L | ||||
| Evaluation Method | Colony-forming assay | ||||
| MOA of PDC |
In this study, we hypothesized that the clinically utilized radiopharmaceutical 68Ga-DOTA-TOC could be converted to a radiolabeled peptide-drug conjugate (PDC) for selective delivery of TMZ to SSTR2-positive tumor cells. We used the intrinsic radiolabeling utility of the PDC to characterize receptor-binding properties, pharmacokinetics (PK), and tissue biodistribution in cells and animal studies. Receptor-targeted DNA-damaging properties and cytotoxic effects of the PDC were examined in different cell lines, and the effects of accumulated doses on MGMT content were evaluated in MGMT-positive cells.
Click to Show/Hide
|
||||
| Description |
TMZ is an alkylating agent that causes cell death through DNA-damaging mechanisms. To determine whether MMC(TMZ)-TOC induces the same cytotoxic effects through a receptor-dependent process, we first studied its DNA-damaging properties in IMR-32 cells that endogenously express SSTR2. We performed an alkaline comet assay to evaluate the ability of our drug conjugate to produce single- and double-stranded DNA breaks. As shown in Figure 3A,B, the targeted agent-induced DNA breaks that were similar to free TMZ, resulting in migrating DNA fragments (comet tail) from the nucleoid (comet head). The damaging effects of MMC(TMZ)-TOC were significantly reduced (P < 0.0001) when cells were preincubated with blocking doses of the high-affinity SSTR2 antagonist JR11, indicating receptor-dependent cytotoxicity. Next, we used a colony formation assay to assess the long-term survival and reproductive capability of the cells after treatment with the PDC. We treated BON1 (receptor-negative) and BON1-SSTR2 (receptor-positive) cells with 2 umol/L MMC(TMZ)-TOC or 10 umol/L TMZ for 5 consecutive days, seeded the cells at a low-density number, and allowed them to grow and form colonies for 14 days. The clonogenic survival data showed that MMC(TMZ)-TOC produced cytotoxic effects in the receptor-positive BON1-SSTR2 cells (P < 0.01) similar to clinically relevant doses of TMZ. Conversely, no cytotoxicity was observed in receptor-negative BON1 cells following treatment with the drug conjugate, further illustrating the receptor-dependent effects of the PDC.
Click to Show/Hide
|
||||
| In Vitro Model | Pancreatic serotonin-producing neuroendocrine tumor | BON-1 cell | CVCL_3985 | ||
References
