Drug Information
General Information of This Drug
| Drug ID | DRG00038 | |||||
|---|---|---|---|---|---|---|
| Drug Name | Monomethyl auristatin E | |||||
| Synonyms |
Monomethyl auristatin E; MMAE; 474645-27-7; Monomethyl auristatin E (vedotin); SCHEMBL16645126; EX-A636; AKOS032947340; D09691
Click to Show/Hide
|
|||||
| Target(s) | Microtubule (MT) | Target Info | ||||
| Structure |
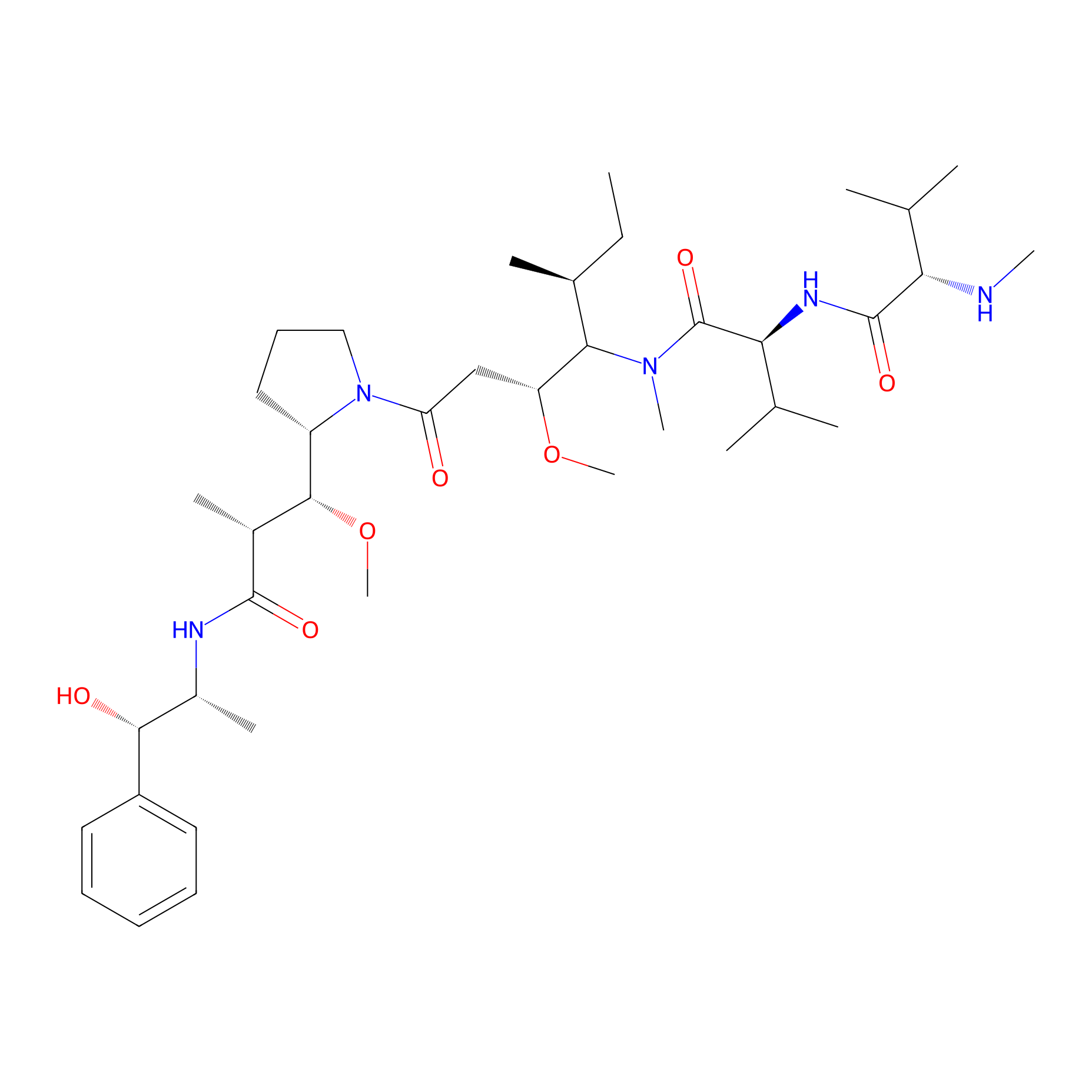
|
|||||
| Formula |
C39H67N5O7
|
|||||
| #Ro5 Violations (Lipinski): 2 | Molecular Weight (mw) | 718 | ||||
| Lipid-water partition coefficient (xlogp) | 4.1 | |||||
| Hydrogen Bond Donor Count (hbonddonor) | 4 | |||||
| Hydrogen Bond Acceptor Count (hbondacc) | 8 | |||||
| Rotatable Bond Count (rotbonds) | 20 | |||||
| PubChem CID | ||||||
| Canonical smiles |
CCC(C)C(C(CC(=O)N1CCCC1C(C(C)C(=O)NC(C)C(C2=CC=CC=C2)O)OC)OC)N(C)C(=O)C(C(C)C)NC(=O)C(C(C)C)NC
|
|||||
| InChI |
InChI=1S/C39H67N5O7/c1-13-25(6)34(43(10)39(49)33(24(4)5)42-38(48)32(40-9)23(2)3)30(50-11)22-31(45)44-21-17-20-29(44)36(51-12)26(7)37(47)41-27(8)35(46)28-18-15-14-16-19-28/h14-16,18-19,23-27,29-30,32-36,40,46H,13,17,20-22H2,1-12H3,(H,41,47)(H,42,48)/t25-,26+,27+,29-,30+,32-,33-,34?,35+,36+/m0/s1
|
|||||
| InChIKey |
DASWEROEPLKSEI-AWNAIHLBSA-N
|
|||||
| IUPAC Name |
(2S)-N-[(2S)-1-[[(3R,5S)-1-[(2S)-2-[(1R,2R)-3-[[(1S,2R)-1-hydroxy-1-phenylpropan-2-yl]amino]-1-methoxy-2-methyl-3-oxopropyl]pyrrolidin-1-yl]-3-methoxy-5-methyl-1-oxoheptan-4-yl]-methylamino]-3-methyl-1-oxobutan-2-yl]-3-methyl-2-(methylamino)butanamide
|
|||||
The activity data of This Drug
| Standard Type | Value | Administration times | Cell line | Cell line ID | Ref. | |
|---|---|---|---|---|---|---|
| Half Maximal Effective Concentration (EC50) | 0.16±0.01 µM | 48 h | MIA PaCa-2 cell | CVCL_0428 | [1] | |
| Half Maximal Effective Concentration (EC50) | 0.14±0.03 nM | 48 h | DX3-puro cell | CVCL_1D33 | [1] | |
| Half Maximal Effective Concentration (EC50) | 0.15±0.02 nM | 48 h | DX3-puro/beta6 cell | CVCL_1D33 | [1] | |
| Half Maximal Effective Concentration (EC50) | 0.50±0.03 nM | 48 h | BxPC-3 (+) cells | CVCL_0186 | [1] | |
| Half Maximal growth inhibition concentration (GI50) | 0.5 nM | 3 days | OVCAR-3 cell | CVCL_0465 | [2] | |
| Half Maximal growth inhibition concentration (GI50) | 0.6 nM | 3 days | H-6036 cell | N.A. | [2] | |
| Half Maximal growth inhibition concentration (GI50) | 0.8 nM | 3 days | SK-OV-3 cell | CVCL_0532 | [2] | |
| Half Maximal growth inhibition concentration (GI50) | 0.8 nM | 3 days | SK-OV-3 cell | CVCL_0532 | [2] | |
| Half Maximal growth inhibition concentration (GI50) | 1.1 nM | 3 days | MRC-5 cell | CVCL_0440 | [2] | |
| Half Maximal Inhibitory Concentration (IC50) | 7.18 nM | 72 h | HGC-27 cell | CVCL_1279 | [3] | |
| Half Maximal Inhibitory Concentration (IC50) | 10.7 nM | 72 h | MKN45 cell | CVCL_0434 | [3] | |
| Half Maximal Inhibitory Concentration (IC50) | 10.97 nM | 72 h | NUGC-4 cell | CVCL_3082 | [3] | |
Each Peptide-drug Conjugate Related to This Drug
Full Information of The Activity Data of The PDC(s) Related to This Drug
BT8009 [Phase 2/3]
Identified from the Human Clinical Data
| Experiment 1 Reporting the Activity Data of This PDC | [4] | ||||
| Indication | Breast cancer | ||||
| Efficacy Data | Tumor Growth Inhibition value (TGI) | 23% | |||
| Administration Time | 28 days | ||||
| Administration Dosage | 1 mg/kg | ||||
| MOA of PDC |
The cell adhesion molecule Nectin-4 shows elevated expression in multiple tumor types correlated with poor prognosis. Nectin-4-directed ADCs show efficacy in multiple xenograft tumor models. The ADC enfortumab vedotin (EV) delivers the antimitotic toxin MMAE to Nectin-4-expressing cells via internalization and cleavage of a valine-citrulline dipeptide linker component. Clinical validation of Nectin-4 as a target in urothelial cancer has been demonstrated with EV. In 2021, the FDA-approved EV for patients with locally advanced or metastatic urothelial cancer who had previously received a PD-1 or PD-L1 inhibitor and platinum-containing chemotherapy or were ineligible for cisplatin containing chemotherapy and had received one or more prior lines of therapy. Bicycle toxin conjugates (BTC) are structurally constrained bicyclic peptides conjugated through cleavable linkers to a toxin. Various, well-described linker toxin combinations can be incorporated into the BTC molecule (e.g., BT1718 and BT5528; refs.). They are of low molecular weight (approximately 4-4.5 kDa) and being chemically synthesized can be optimized for appropriate affinity, stability, and solubility relatively simply. Through intravenous administration, high systemic Cmax values can be attained, which, along with BTCs relatively small size, helps drive rapid diffusion into extra-vascular compartment, as reflected in a volume of distribution similar to extracellular fluid. We believe that delivery of a high number of BTCs, each carrying a reduced toxin load (peptide toxin ratio of 1:1) should improve tumor penetration and reduce the impact of the binding site barrier. BTCs show moderate clearance from the systemic vasculature, predominantly by the renal route. This overall profile marks them out from most ADCs and provides the possibility of enhanced clinical efficacy with a wider therapeutic index. BTCs are new therapeutic modality that shows a very different pharmacokinetic and structural profile to classic ADCs, whereas possessing robust tumoricidal properties. BTCs targeting MT1-MMP and EphA2 are currently in clinical trials. BT8009 is the most recent BTC to enter clinical trial. BT8009 is highly selective for Nectin-4 over other nectin family members and an extensive range of cell membrane expressed proteins. It shares the same cleavable linker and toxin combination as EV and can be cleaved by proteases in the TME, releasing cell penetrant MMAE that diffuses into tumor cells, or bystander stromal-supportive cells, evoking cell death, and tumor regression. It shows a robust and dose-dependent antitumor activity in multiple CDX and PDX models, representing lung, breast, bladder, head and neck cancers. Optimal tumor regression is associated with membrane expression of Nectin-4, in conjunction with MMAE sensitivity. Tumor regression rates are comparable for small and large tumors, indicative of deep and rapid penetration throughout the tumor. BT8009 provides tumoricidal activity with several regimens, potentially allowing for clinical titration of dose and dose interval if required.
Click to Show/Hide
|
||||
| Description |
BT8009 demonstrated dose-related effects on tumor growth in CDX and PDX models over the range 1-3 mg/kg when administered qw. Full tumor regressions were routinely achieved in both models with 3 mg/kg, with no tumor regrowth in subsequent weeks off treatment. Stable disease was delivered by 2 mg/kg and at this dose, in the PDX model, tumor growth resumed after drug cessation. In both models animals from the vehicle treated group were treated with 3 mg/kg BT8009 when tumors reached approximately 800 mm3or 1,000 mm3. Profound tumor regression was rapidly initiated in response. In the majority of studies 3 mg/kg, qw, was adopted as the standard dosing regimen.
Click to Show/Hide
|
||||
| In Vivo Model | BALB/c nude mice non-small cell lung cell-derived xenograft model. | ||||
| Half life period | 1-2 h | ||||
| Experiment 2 Reporting the Activity Data of This PDC | [4] | ||||
| Indication | Breast cancer | ||||
| Efficacy Data | Tumor Growth Inhibition value (TGI) | 60% | |||
| Administration Time | 28 days | ||||
| Administration Dosage | 1 mg/kg | ||||
| MOA of PDC |
The cell adhesion molecule Nectin-4 shows elevated expression in multiple tumor types correlated with poor prognosis. Nectin-4-directed ADCs show efficacy in multiple xenograft tumor models. The ADC enfortumab vedotin (EV) delivers the antimitotic toxin MMAE to Nectin-4-expressing cells via internalization and cleavage of a valine-citrulline dipeptide linker component. Clinical validation of Nectin-4 as a target in urothelial cancer has been demonstrated with EV. In 2021, the FDA-approved EV for patients with locally advanced or metastatic urothelial cancer who had previously received a PD-1 or PD-L1 inhibitor and platinum-containing chemotherapy or were ineligible for cisplatin containing chemotherapy and had received one or more prior lines of therapy. Bicycle toxin conjugates (BTC) are structurally constrained bicyclic peptides conjugated through cleavable linkers to a toxin. Various, well-described linker toxin combinations can be incorporated into the BTC molecule (e.g., BT1718 and BT5528; refs.). They are of low molecular weight (approximately 4-4.5 kDa) and being chemically synthesized can be optimized for appropriate affinity, stability, and solubility relatively simply. Through intravenous administration, high systemic Cmax values can be attained, which, along with BTCs relatively small size, helps drive rapid diffusion into extra-vascular compartment, as reflected in a volume of distribution similar to extracellular fluid. We believe that delivery of a high number of BTCs, each carrying a reduced toxin load (peptide toxin ratio of 1:1) should improve tumor penetration and reduce the impact of the binding site barrier. BTCs show moderate clearance from the systemic vasculature, predominantly by the renal route. This overall profile marks them out from most ADCs and provides the possibility of enhanced clinical efficacy with a wider therapeutic index. BTCs are new therapeutic modality that shows a very different pharmacokinetic and structural profile to classic ADCs, whereas possessing robust tumoricidal properties. BTCs targeting MT1-MMP and EphA2 are currently in clinical trials. BT8009 is the most recent BTC to enter clinical trial. BT8009 is highly selective for Nectin-4 over other nectin family members and an extensive range of cell membrane expressed proteins. It shares the same cleavable linker and toxin combination as EV and can be cleaved by proteases in the TME, releasing cell penetrant MMAE that diffuses into tumor cells, or bystander stromal-supportive cells, evoking cell death, and tumor regression. It shows a robust and dose-dependent antitumor activity in multiple CDX and PDX models, representing lung, breast, bladder, head and neck cancers. Optimal tumor regression is associated with membrane expression of Nectin-4, in conjunction with MMAE sensitivity. Tumor regression rates are comparable for small and large tumors, indicative of deep and rapid penetration throughout the tumor. BT8009 provides tumoricidal activity with several regimens, potentially allowing for clinical titration of dose and dose interval if required.
Click to Show/Hide
|
||||
| Description |
BT8009 demonstrated dose-related effects on tumor growth in CDX and PDX models over the range 1-3 mg/kg when administered qw. Full tumor regressions were routinely achieved in both models with 3 mg/kg, with no tumor regrowth in subsequent weeks off treatment. Stable disease was delivered by 2 mg/kg and at this dose, in the PDX model, tumor growth resumed after drug cessation. In both models animals from the vehicle treated group were treated with 3 mg/kg BT8009 when tumors reached approximately 800 mm3or 1,000 mm3. Profound tumor regression was rapidly initiated in response. In the majority of studies 3 mg/kg, qw, was adopted as the standard dosing regimen.
Click to Show/Hide
|
||||
| In Vivo Model | BALB/c nude mice triple-negative breast cancer cell-derived xenograft model. | ||||
| Half life period | 1-2 h | ||||
| Experiment 3 Reporting the Activity Data of This PDC | [4] | ||||
| Indication | Breast cancer | ||||
| Efficacy Data | Tumor Growth Inhibition value (TGI) | 74% | |||
| Administration Time | 28 days | ||||
| Administration Dosage | 2 mg/kg | ||||
| MOA of PDC |
The cell adhesion molecule Nectin-4 shows elevated expression in multiple tumor types correlated with poor prognosis. Nectin-4-directed ADCs show efficacy in multiple xenograft tumor models. The ADC enfortumab vedotin (EV) delivers the antimitotic toxin MMAE to Nectin-4-expressing cells via internalization and cleavage of a valine-citrulline dipeptide linker component. Clinical validation of Nectin-4 as a target in urothelial cancer has been demonstrated with EV. In 2021, the FDA-approved EV for patients with locally advanced or metastatic urothelial cancer who had previously received a PD-1 or PD-L1 inhibitor and platinum-containing chemotherapy or were ineligible for cisplatin containing chemotherapy and had received one or more prior lines of therapy. Bicycle toxin conjugates (BTC) are structurally constrained bicyclic peptides conjugated through cleavable linkers to a toxin. Various, well-described linker toxin combinations can be incorporated into the BTC molecule (e.g., BT1718 and BT5528; refs.). They are of low molecular weight (approximately 4-4.5 kDa) and being chemically synthesized can be optimized for appropriate affinity, stability, and solubility relatively simply. Through intravenous administration, high systemic Cmax values can be attained, which, along with BTCs relatively small size, helps drive rapid diffusion into extra-vascular compartment, as reflected in a volume of distribution similar to extracellular fluid. We believe that delivery of a high number of BTCs, each carrying a reduced toxin load (peptide toxin ratio of 1:1) should improve tumor penetration and reduce the impact of the binding site barrier. BTCs show moderate clearance from the systemic vasculature, predominantly by the renal route. This overall profile marks them out from most ADCs and provides the possibility of enhanced clinical efficacy with a wider therapeutic index. BTCs are new therapeutic modality that shows a very different pharmacokinetic and structural profile to classic ADCs, whereas possessing robust tumoricidal properties. BTCs targeting MT1-MMP and EphA2 are currently in clinical trials. BT8009 is the most recent BTC to enter clinical trial. BT8009 is highly selective for Nectin-4 over other nectin family members and an extensive range of cell membrane expressed proteins. It shares the same cleavable linker and toxin combination as EV and can be cleaved by proteases in the TME, releasing cell penetrant MMAE that diffuses into tumor cells, or bystander stromal-supportive cells, evoking cell death, and tumor regression. It shows a robust and dose-dependent antitumor activity in multiple CDX and PDX models, representing lung, breast, bladder, head and neck cancers. Optimal tumor regression is associated with membrane expression of Nectin-4, in conjunction with MMAE sensitivity. Tumor regression rates are comparable for small and large tumors, indicative of deep and rapid penetration throughout the tumor. BT8009 provides tumoricidal activity with several regimens, potentially allowing for clinical titration of dose and dose interval if required.
Click to Show/Hide
|
||||
| Description |
BT8009 demonstrated dose-related effects on tumor growth in CDX and PDX models over the range 1-3 mg/kg when administered qw. Full tumor regressions were routinely achieved in both models with 3 mg/kg, with no tumor regrowth in subsequent weeks off treatment. Stable disease was delivered by 2 mg/kg and at this dose, in the PDX model, tumor growth resumed after drug cessation. In both models animals from the vehicle treated group were treated with 3 mg/kg BT8009 when tumors reached approximately 800 mm3or 1,000 mm3. Profound tumor regression was rapidly initiated in response. In the majority of studies 3 mg/kg, qw, was adopted as the standard dosing regimen.
Click to Show/Hide
|
||||
| In Vivo Model | BALB/c nude mice triple-negative breast cancer cell-derived xenograft model. | ||||
| Half life period | 1-2 h | ||||
| Experiment 4 Reporting the Activity Data of This PDC | [4] | ||||
| Indication | Breast cancer | ||||
| Efficacy Data | Tumor Growth Inhibition value (TGI) | 77% | |||
| Administration Time | 28 days | ||||
| Administration Dosage | 2 mg/kg | ||||
| MOA of PDC |
The cell adhesion molecule Nectin-4 shows elevated expression in multiple tumor types correlated with poor prognosis. Nectin-4-directed ADCs show efficacy in multiple xenograft tumor models. The ADC enfortumab vedotin (EV) delivers the antimitotic toxin MMAE to Nectin-4-expressing cells via internalization and cleavage of a valine-citrulline dipeptide linker component. Clinical validation of Nectin-4 as a target in urothelial cancer has been demonstrated with EV. In 2021, the FDA-approved EV for patients with locally advanced or metastatic urothelial cancer who had previously received a PD-1 or PD-L1 inhibitor and platinum-containing chemotherapy or were ineligible for cisplatin containing chemotherapy and had received one or more prior lines of therapy. Bicycle toxin conjugates (BTC) are structurally constrained bicyclic peptides conjugated through cleavable linkers to a toxin. Various, well-described linker toxin combinations can be incorporated into the BTC molecule (e.g., BT1718 and BT5528; refs.). They are of low molecular weight (approximately 4-4.5 kDa) and being chemically synthesized can be optimized for appropriate affinity, stability, and solubility relatively simply. Through intravenous administration, high systemic Cmax values can be attained, which, along with BTCs relatively small size, helps drive rapid diffusion into extra-vascular compartment, as reflected in a volume of distribution similar to extracellular fluid. We believe that delivery of a high number of BTCs, each carrying a reduced toxin load (peptide toxin ratio of 1:1) should improve tumor penetration and reduce the impact of the binding site barrier. BTCs show moderate clearance from the systemic vasculature, predominantly by the renal route. This overall profile marks them out from most ADCs and provides the possibility of enhanced clinical efficacy with a wider therapeutic index. BTCs are new therapeutic modality that shows a very different pharmacokinetic and structural profile to classic ADCs, whereas possessing robust tumoricidal properties. BTCs targeting MT1-MMP and EphA2 are currently in clinical trials. BT8009 is the most recent BTC to enter clinical trial. BT8009 is highly selective for Nectin-4 over other nectin family members and an extensive range of cell membrane expressed proteins. It shares the same cleavable linker and toxin combination as EV and can be cleaved by proteases in the TME, releasing cell penetrant MMAE that diffuses into tumor cells, or bystander stromal-supportive cells, evoking cell death, and tumor regression. It shows a robust and dose-dependent antitumor activity in multiple CDX and PDX models, representing lung, breast, bladder, head and neck cancers. Optimal tumor regression is associated with membrane expression of Nectin-4, in conjunction with MMAE sensitivity. Tumor regression rates are comparable for small and large tumors, indicative of deep and rapid penetration throughout the tumor. BT8009 provides tumoricidal activity with several regimens, potentially allowing for clinical titration of dose and dose interval if required.
Click to Show/Hide
|
||||
| Description |
BT8009 demonstrated dose-related effects on tumor growth in CDX and PDX models over the range 1-3 mg/kg when administered qw. Full tumor regressions were routinely achieved in both models with 3 mg/kg, with no tumor regrowth in subsequent weeks off treatment. Stable disease was delivered by 2 mg/kg and at this dose, in the PDX model, tumor growth resumed after drug cessation. In both models animals from the vehicle treated group were treated with 3 mg/kg BT8009 when tumors reached approximately 800 mm3or 1,000 mm3. Profound tumor regression was rapidly initiated in response. In the majority of studies 3 mg/kg, qw, was adopted as the standard dosing regimen.
Click to Show/Hide
|
||||
| In Vivo Model | BALB/c nude mice non-small cell lung cell-derived xenograft model. | ||||
| Half life period | 1-2 h | ||||
| Experiment 5 Reporting the Activity Data of This PDC | [4] | ||||
| Indication | Breast cancer | ||||
| Efficacy Data | Tumor Growth Inhibition value (TGI) | 96% | |||
| Administration Time | 28 days | ||||
| Administration Dosage | 3 mg/kg | ||||
| MOA of PDC |
The cell adhesion molecule Nectin-4 shows elevated expression in multiple tumor types correlated with poor prognosis. Nectin-4-directed ADCs show efficacy in multiple xenograft tumor models. The ADC enfortumab vedotin (EV) delivers the antimitotic toxin MMAE to Nectin-4-expressing cells via internalization and cleavage of a valine-citrulline dipeptide linker component. Clinical validation of Nectin-4 as a target in urothelial cancer has been demonstrated with EV. In 2021, the FDA-approved EV for patients with locally advanced or metastatic urothelial cancer who had previously received a PD-1 or PD-L1 inhibitor and platinum-containing chemotherapy or were ineligible for cisplatin containing chemotherapy and had received one or more prior lines of therapy. Bicycle toxin conjugates (BTC) are structurally constrained bicyclic peptides conjugated through cleavable linkers to a toxin. Various, well-described linker toxin combinations can be incorporated into the BTC molecule (e.g., BT1718 and BT5528; refs.). They are of low molecular weight (approximately 4-4.5 kDa) and being chemically synthesized can be optimized for appropriate affinity, stability, and solubility relatively simply. Through intravenous administration, high systemic Cmax values can be attained, which, along with BTCs relatively small size, helps drive rapid diffusion into extra-vascular compartment, as reflected in a volume of distribution similar to extracellular fluid. We believe that delivery of a high number of BTCs, each carrying a reduced toxin load (peptide toxin ratio of 1:1) should improve tumor penetration and reduce the impact of the binding site barrier. BTCs show moderate clearance from the systemic vasculature, predominantly by the renal route. This overall profile marks them out from most ADCs and provides the possibility of enhanced clinical efficacy with a wider therapeutic index. BTCs are new therapeutic modality that shows a very different pharmacokinetic and structural profile to classic ADCs, whereas possessing robust tumoricidal properties. BTCs targeting MT1-MMP and EphA2 are currently in clinical trials. BT8009 is the most recent BTC to enter clinical trial. BT8009 is highly selective for Nectin-4 over other nectin family members and an extensive range of cell membrane expressed proteins. It shares the same cleavable linker and toxin combination as EV and can be cleaved by proteases in the TME, releasing cell penetrant MMAE that diffuses into tumor cells, or bystander stromal-supportive cells, evoking cell death, and tumor regression. It shows a robust and dose-dependent antitumor activity in multiple CDX and PDX models, representing lung, breast, bladder, head and neck cancers. Optimal tumor regression is associated with membrane expression of Nectin-4, in conjunction with MMAE sensitivity. Tumor regression rates are comparable for small and large tumors, indicative of deep and rapid penetration throughout the tumor. BT8009 provides tumoricidal activity with several regimens, potentially allowing for clinical titration of dose and dose interval if required.
Click to Show/Hide
|
||||
| Description |
BT8009 demonstrated dose-related effects on tumor growth in CDX and PDX models over the range 1-3 mg/kg when administered qw. Full tumor regressions were routinely achieved in both models with 3 mg/kg, with no tumor regrowth in subsequent weeks off treatment. Stable disease was delivered by 2 mg/kg and at this dose, in the PDX model, tumor growth resumed after drug cessation. In both models animals from the vehicle treated group were treated with 3 mg/kg BT8009 when tumors reached approximately 800 mm3or 1,000 mm3. Profound tumor regression was rapidly initiated in response. In the majority of studies 3 mg/kg, qw, was adopted as the standard dosing regimen.
Click to Show/Hide
|
||||
| In Vivo Model | BALB/c nude mice triple-negative breast cancer cell-derived xenograft model. | ||||
| Half life period | 1-2 h | ||||
| Experiment 6 Reporting the Activity Data of This PDC | [4] | ||||
| Indication | Breast cancer | ||||
| Efficacy Data | Tumor Growth Inhibition value (TGI) | 98% | |||
| Administration Time | 28 days | ||||
| Administration Dosage | 3 mg/kg | ||||
| MOA of PDC |
The cell adhesion molecule Nectin-4 shows elevated expression in multiple tumor types correlated with poor prognosis. Nectin-4-directed ADCs show efficacy in multiple xenograft tumor models. The ADC enfortumab vedotin (EV) delivers the antimitotic toxin MMAE to Nectin-4-expressing cells via internalization and cleavage of a valine-citrulline dipeptide linker component. Clinical validation of Nectin-4 as a target in urothelial cancer has been demonstrated with EV. In 2021, the FDA-approved EV for patients with locally advanced or metastatic urothelial cancer who had previously received a PD-1 or PD-L1 inhibitor and platinum-containing chemotherapy or were ineligible for cisplatin containing chemotherapy and had received one or more prior lines of therapy. Bicycle toxin conjugates (BTC) are structurally constrained bicyclic peptides conjugated through cleavable linkers to a toxin. Various, well-described linker toxin combinations can be incorporated into the BTC molecule (e.g., BT1718 and BT5528; refs.). They are of low molecular weight (approximately 4-4.5 kDa) and being chemically synthesized can be optimized for appropriate affinity, stability, and solubility relatively simply. Through intravenous administration, high systemic Cmax values can be attained, which, along with BTCs relatively small size, helps drive rapid diffusion into extra-vascular compartment, as reflected in a volume of distribution similar to extracellular fluid. We believe that delivery of a high number of BTCs, each carrying a reduced toxin load (peptide toxin ratio of 1:1) should improve tumor penetration and reduce the impact of the binding site barrier. BTCs show moderate clearance from the systemic vasculature, predominantly by the renal route. This overall profile marks them out from most ADCs and provides the possibility of enhanced clinical efficacy with a wider therapeutic index. BTCs are new therapeutic modality that shows a very different pharmacokinetic and structural profile to classic ADCs, whereas possessing robust tumoricidal properties. BTCs targeting MT1-MMP and EphA2 are currently in clinical trials. BT8009 is the most recent BTC to enter clinical trial. BT8009 is highly selective for Nectin-4 over other nectin family members and an extensive range of cell membrane expressed proteins. It shares the same cleavable linker and toxin combination as EV and can be cleaved by proteases in the TME, releasing cell penetrant MMAE that diffuses into tumor cells, or bystander stromal-supportive cells, evoking cell death, and tumor regression. It shows a robust and dose-dependent antitumor activity in multiple CDX and PDX models, representing lung, breast, bladder, head and neck cancers. Optimal tumor regression is associated with membrane expression of Nectin-4, in conjunction with MMAE sensitivity. Tumor regression rates are comparable for small and large tumors, indicative of deep and rapid penetration throughout the tumor. BT8009 provides tumoricidal activity with several regimens, potentially allowing for clinical titration of dose and dose interval if required.
Click to Show/Hide
|
||||
| Description |
BT8009 demonstrated dose-related effects on tumor growth in CDX and PDX models over the range 1-3 mg/kg when administered qw. Full tumor regressions were routinely achieved in both models with 3 mg/kg, with no tumor regrowth in subsequent weeks off treatment. Stable disease was delivered by 2 mg/kg and at this dose, in the PDX model, tumor growth resumed after drug cessation. In both models animals from the vehicle treated group were treated with 3 mg/kg BT8009 when tumors reached approximately 800 mm3or 1,000 mm3. Profound tumor regression was rapidly initiated in response. In the majority of studies 3 mg/kg, qw, was adopted as the standard dosing regimen.
Click to Show/Hide
|
||||
| In Vivo Model | BALB/c nude mice non-small cell lung cell-derived xenograft model. | ||||
| Half life period | 1-2 h | ||||
Discovered Using Cell Line-derived Xenograft Model
| Experiment 1 Reporting the Activity Data of This PDC | [6] | ||||
| Indication | Breast cancer | ||||
| Efficacy Data | Tumor Growth Inhibition value (TGI) | 81% | |||
| Administration Time | 21 days | ||||
| Administration Dosage | 3 mg/kg qw | ||||
| MOA of PDC |
Nectin-4 is a cell adhesion molecule from the Nectin and Nectin-like family. It is a clinically validated tumor target and has been reported to be highly expressed in a wide range of solid tumors, including bladder, esophageal, pancreatic, and lung, but with limited distribution in healthy tissues.An antibody drug conjugate (PADCEV, enfortumab vedotin) that targets Nectin-4 was recently approved for the treatment of bladder cancer following the generation of positive data in a number of clinical studies. Herein we describe the discovery via phage display and subsequent chemical optimization of a Nectin-4 binding Bicycle and its incorporation into BT8009, a BTC that is currently under clinical evaluation. A detailed report of the pharmacologic properties of BT8009 has recently been described.In this, BT8009 shows potent efficacy in multiple tumor models, including patient-derived xenografts, across a variety of tumor indications and is well-tolerated in preclinical safety studies. In several models it demonstrated superior or equivalent efficacy to an analogue of the ADC PADCEV.
Click to Show/Hide
|
||||
| Description |
The efficacy of BT8009 was evaluated in a cell-derived xenograft (CDX) model using breast adenocarcinoma (MDA-MB-468) cells, which express Nectin-4.When tested at a dose of 3 mg/kg once weekly, significant antitumor activity was observed. At a dose of 3 mg/kg twice weekly or 5 mg/kg once weekly, potent efficacy was achieved with almost complete regression of the tumor after 18 days. Importantly, following cessation of dosing after 18 days, animals from the 5 mg/kg once weekly dosing group were monitored up to day 42, and no tumor regrowth was observed. Consistent animal body weights throughout the study indicate that BT8009 appeared to be well-tolerated at all doses tested. In additional studies reported elsewhere, BT8009 has shown preclinical efficacy in a wide range of CDX and PDX tumor types with full tumor regression seen in small and large tumors, where efficacy broadly correlates with Nectin-4 expression. Additionally, when BT8009 was codosed with an excess of an MMAE-free analogue, efficacy was attenuated, and a BTC incorporating a nonbinding Bicycle analogue showed a demonstrably lower rate and degree of tumor regression.
Click to Show/Hide
|
||||
| In Vivo Model | MDA-MB-468 cell-derived xenograft (CDX) model. | ||||
| In Vitro Model | Breast adenocarcinoma | MDA-MB-468 cell | CVCL_0419 | ||
| Experiment 2 Reporting the Activity Data of This PDC | [6] | ||||
| Indication | Breast cancer | ||||
| Efficacy Data | Tumor Growth Inhibition value (TGI) | 93% | |||
| Administration Time | 21 days | ||||
| Administration Dosage | 3 mg/kg biw | ||||
| MOA of PDC |
Nectin-4 is a cell adhesion molecule from the Nectin and Nectin-like family. It is a clinically validated tumor target and has been reported to be highly expressed in a wide range of solid tumors, including bladder, esophageal, pancreatic, and lung, but with limited distribution in healthy tissues.An antibody drug conjugate (PADCEV, enfortumab vedotin) that targets Nectin-4 was recently approved for the treatment of bladder cancer following the generation of positive data in a number of clinical studies. Herein we describe the discovery via phage display and subsequent chemical optimization of a Nectin-4 binding Bicycle and its incorporation into BT8009, a BTC that is currently under clinical evaluation. A detailed report of the pharmacologic properties of BT8009 has recently been described.In this, BT8009 shows potent efficacy in multiple tumor models, including patient-derived xenografts, across a variety of tumor indications and is well-tolerated in preclinical safety studies. In several models it demonstrated superior or equivalent efficacy to an analogue of the ADC PADCEV.
Click to Show/Hide
|
||||
| Description |
The efficacy of BT8009 was evaluated in a cell-derived xenograft (CDX) model using breast adenocarcinoma (MDA-MB-468) cells, which express Nectin-4.When tested at a dose of 3 mg/kg once weekly, significant antitumor activity was observed. At a dose of 3 mg/kg twice weekly or 5 mg/kg once weekly, potent efficacy was achieved with almost complete regression of the tumor after 18 days. Importantly, following cessation of dosing after 18 days, animals from the 5 mg/kg once weekly dosing group were monitored up to day 42, and no tumor regrowth was observed. Consistent animal body weights throughout the study indicate that BT8009 appeared to be well-tolerated at all doses tested. In additional studies reported elsewhere, BT8009 has shown preclinical efficacy in a wide range of CDX and PDX tumor types with full tumor regression seen in small and large tumors, where efficacy broadly correlates with Nectin-4 expression. Additionally, when BT8009 was codosed with an excess of an MMAE-free analogue, efficacy was attenuated, and a BTC incorporating a nonbinding Bicycle analogue showed a demonstrably lower rate and degree of tumor regression.
Click to Show/Hide
|
||||
| In Vivo Model | MDA-MB-468 cell-derived xenograft (CDX) model. | ||||
| In Vitro Model | Breast adenocarcinoma | MDA-MB-468 cell | CVCL_0419 | ||
| Experiment 3 Reporting the Activity Data of This PDC | [6] | ||||
| Indication | Breast cancer | ||||
| Efficacy Data | Tumor Growth Inhibition value (TGI) | 93% | |||
| Administration Time | 21 days | ||||
| Administration Dosage | 5 mg/kg qw | ||||
| MOA of PDC |
Nectin-4 is a cell adhesion molecule from the Nectin and Nectin-like family. It is a clinically validated tumor target and has been reported to be highly expressed in a wide range of solid tumors, including bladder, esophageal, pancreatic, and lung, but with limited distribution in healthy tissues.An antibody drug conjugate (PADCEV, enfortumab vedotin) that targets Nectin-4 was recently approved for the treatment of bladder cancer following the generation of positive data in a number of clinical studies. Herein we describe the discovery via phage display and subsequent chemical optimization of a Nectin-4 binding Bicycle and its incorporation into BT8009, a BTC that is currently under clinical evaluation. A detailed report of the pharmacologic properties of BT8009 has recently been described.In this, BT8009 shows potent efficacy in multiple tumor models, including patient-derived xenografts, across a variety of tumor indications and is well-tolerated in preclinical safety studies. In several models it demonstrated superior or equivalent efficacy to an analogue of the ADC PADCEV.
Click to Show/Hide
|
||||
| Description |
The efficacy of BT8009 was evaluated in a cell-derived xenograft (CDX) model using breast adenocarcinoma (MDA-MB-468) cells, which express Nectin-4.When tested at a dose of 3 mg/kg once weekly, significant antitumor activity was observed. At a dose of 3 mg/kg twice weekly or 5 mg/kg once weekly, potent efficacy was achieved with almost complete regression of the tumor after 18 days. Importantly, following cessation of dosing after 18 days, animals from the 5 mg/kg once weekly dosing group were monitored up to day 42, and no tumor regrowth was observed. Consistent animal body weights throughout the study indicate that BT8009 appeared to be well-tolerated at all doses tested. In additional studies reported elsewhere, BT8009 has shown preclinical efficacy in a wide range of CDX and PDX tumor types with full tumor regression seen in small and large tumors, where efficacy broadly correlates with Nectin-4 expression. Additionally, when BT8009 was codosed with an excess of an MMAE-free analogue, efficacy was attenuated, and a BTC incorporating a nonbinding Bicycle analogue showed a demonstrably lower rate and degree of tumor regression.
Click to Show/Hide
|
||||
| In Vivo Model | MDA-MB-468 cell-derived xenograft (CDX) model. | ||||
| In Vitro Model | Breast adenocarcinoma | MDA-MB-468 cell | CVCL_0419 | ||
CBP-1008 [Phase 2/3]
Identified from the Human Clinical Data
| Experiment 1 Reporting the Activity Data of This PDC | [5] | ||||
| Indication | Ovarian clear cell carcinoma | ||||
| Efficacy Data | Stable disease (SD) | 31.30% | |||
| Patients Enrolled |
16 platinum-resistant ovarian clear cell carcinoma patients.
|
||||
| Administration Dosage | 0.15 mg/kg | ||||
| MOA of PDC |
Folate receptor α (FRα) and vanilloid subfamily member 6 of transient receptor potential channels (TRPV6) are potential promising therapeutic targets due to their high expression level in many solid tumors including ovarian cancer. CBP-1008 is a first-in-class (FIC) bi-specific ligand drug conjugate targeting FRα and TRPV6 carrying monomethyl auristatin E (MMAE) as payload.
Click to Show/Hide
|
||||
| Description |
OCCC accounts for 5% to 25% of OC1, and current treatment options have very poor ORR of <10%. The ORR of CBP-1008 (0.15 or 0.17 mg/kg) for OCCC patients was 31.3% (5/16), regardless of FR expression.
|
||||
| Experiment 2 Reporting the Activity Data of This PDC | [5] | ||||
| Indication | Ovarian cancer | ||||
| Efficacy Data | Stable disease (SD) | 34.50% | |||
| Patients Enrolled |
29 platinum-resistant ovarian cancer patients.
|
||||
| Administration Dosage | 0.15 mg/kg | ||||
| MOA of PDC |
Folate receptor α (FRα) and vanilloid subfamily member 6 of transient receptor potential channels (TRPV6) are potential promising therapeutic targets due to their high expression level in many solid tumors including ovarian cancer. CBP-1008 is a first-in-class (FIC) bi-specific ligand drug conjugate targeting FRα and TRPV6 carrying monomethyl auristatin E (MMAE) as payload.
Click to Show/Hide
|
||||
| Description |
Promising efficacy was observed in HGSOC patients (pts) who received prior 1-2L of TIT (if prior 2L, ≥12m of time interval between 2L; and ≥3m of time interval from the last TIT to CBP-1008 first dose). The ORR is 48.3%(14/29) and DCR is 82.8%(24/29), regardless of FR expression.
|
||||
| Experiment 3 Reporting the Activity Data of This PDC | [5] | ||||
| Indication | Ovarian cancer | ||||
| Efficacy Data | Progressive disease (PD) | 17.20% | |||
| Patients Enrolled |
29 platinum-resistant ovarian cancer patients.
|
||||
| Administration Dosage | 0.15 mg/kg | ||||
| MOA of PDC |
Folate receptor α (FRα) and vanilloid subfamily member 6 of transient receptor potential channels (TRPV6) are potential promising therapeutic targets due to their high expression level in many solid tumors including ovarian cancer. CBP-1008 is a first-in-class (FIC) bi-specific ligand drug conjugate targeting FRα and TRPV6 carrying monomethyl auristatin E (MMAE) as payload.
Click to Show/Hide
|
||||
| Description |
Promising efficacy was observed in HGSOC patients (pts) who received prior 1-2L of TIT (if prior 2L, ≥12m of time interval between 2L; and ≥3m of time interval from the last TIT to CBP-1008 first dose). The ORR is 48.3%(14/29) and DCR is 82.8%(24/29), regardless of FR expression.
|
||||
| Experiment 4 Reporting the Activity Data of This PDC | [5] | ||||
| Indication | Ovarian clear cell carcinoma | ||||
| Efficacy Data | Progressive disease (PD) | 37.40% | |||
| Patients Enrolled |
16 platinum-resistant ovarian clear cell carcinoma patients.
|
||||
| Administration Dosage | 0.15 mg/kg | ||||
| MOA of PDC |
Folate receptor α (FRα) and vanilloid subfamily member 6 of transient receptor potential channels (TRPV6) are potential promising therapeutic targets due to their high expression level in many solid tumors including ovarian cancer. CBP-1008 is a first-in-class (FIC) bi-specific ligand drug conjugate targeting FRα and TRPV6 carrying monomethyl auristatin E (MMAE) as payload.
Click to Show/Hide
|
||||
| Description |
OCCC accounts for 5% to 25% of OC1, and current treatment options have very poor ORR of <10%. The ORR of CBP-1008 (0.15 or 0.17 mg/kg) for OCCC patients was 31.3% (5/16), regardless of FR expression.
|
||||
| Experiment 5 Reporting the Activity Data of This PDC | [5] | ||||
| Indication | Ovarian clear cell carcinoma | ||||
| Efficacy Data | Partial response (PR) | 31.30% | |||
| Patients Enrolled |
16 platinum-resistant ovarian clear cell carcinoma patients.
|
||||
| Administration Dosage | 0.15 mg/kg | ||||
| MOA of PDC |
Folate receptor α (FRα) and vanilloid subfamily member 6 of transient receptor potential channels (TRPV6) are potential promising therapeutic targets due to their high expression level in many solid tumors including ovarian cancer. CBP-1008 is a first-in-class (FIC) bi-specific ligand drug conjugate targeting FRα and TRPV6 carrying monomethyl auristatin E (MMAE) as payload.
Click to Show/Hide
|
||||
| Description |
OCCC accounts for 5% to 25% of OC1, and current treatment options have very poor ORR of <10%. The ORR of CBP-1008 (0.15 or 0.17 mg/kg) for OCCC patients was 31.3% (5/16), regardless of FR expression.
|
||||
| Experiment 6 Reporting the Activity Data of This PDC | [5] | ||||
| Indication | Ovarian cancer | ||||
| Efficacy Data | Partial response (PR) | 48.30% | |||
| Patients Enrolled |
29 platinum-resistant ovarian cancer patients.
|
||||
| Administration Dosage | 0.15 mg/kg | ||||
| MOA of PDC |
Folate receptor α (FRα) and vanilloid subfamily member 6 of transient receptor potential channels (TRPV6) are potential promising therapeutic targets due to their high expression level in many solid tumors including ovarian cancer. CBP-1008 is a first-in-class (FIC) bi-specific ligand drug conjugate targeting FRα and TRPV6 carrying monomethyl auristatin E (MMAE) as payload.
Click to Show/Hide
|
||||
| Description |
Promising efficacy was observed in HGSOC patients (pts) who received prior 1-2L of TIT (if prior 2L, ≥12m of time interval between 2L; and ≥3m of time interval from the last TIT to CBP-1008 first dose). The ORR is 48.3%(14/29) and DCR is 82.8%(24/29), regardless of FR expression.
|
||||
| Experiment 7 Reporting the Activity Data of This PDC | [5] | ||||
| Indication | Ovarian clear cell carcinoma | ||||
| Efficacy Data | Objective response rate(ORR) | 31.30% | |||
| Patients Enrolled |
16 platinum-resistant ovarian clear cell carcinoma patients.
|
||||
| Administration Dosage | 0.15 mg/kg | ||||
| MOA of PDC |
Folate receptor α (FRα) and vanilloid subfamily member 6 of transient receptor potential channels (TRPV6) are potential promising therapeutic targets due to their high expression level in many solid tumors including ovarian cancer. CBP-1008 is a first-in-class (FIC) bi-specific ligand drug conjugate targeting FRα and TRPV6 carrying monomethyl auristatin E (MMAE) as payload.
Click to Show/Hide
|
||||
| Description |
OCCC accounts for 5% to 25% of OC1, and current treatment options have very poor ORR of <10%. The ORR of CBP-1008 (0.15 or 0.17 mg/kg) for OCCC patients was 31.3% (5/16), regardless of FR expression.
|
||||
| Experiment 8 Reporting the Activity Data of This PDC | [5] | ||||
| Indication | Ovarian cancer | ||||
| Efficacy Data | Objective response rate(ORR) | 48.30% | |||
| Patients Enrolled |
29 platinum-resistant ovarian cancer patients.
|
||||
| Administration Dosage | 0.15 mg/kg | ||||
| MOA of PDC |
Folate receptor α (FRα) and vanilloid subfamily member 6 of transient receptor potential channels (TRPV6) are potential promising therapeutic targets due to their high expression level in many solid tumors including ovarian cancer. CBP-1008 is a first-in-class (FIC) bi-specific ligand drug conjugate targeting FRα and TRPV6 carrying monomethyl auristatin E (MMAE) as payload.
Click to Show/Hide
|
||||
| Description |
Promising efficacy was observed in HGSOC patients (pts) who received prior 1-2L of TIT (if prior 2L, ≥12m of time interval between 2L; and ≥3m of time interval from the last TIT to CBP-1008 first dose). The ORR is 48.3%(14/29) and DCR is 82.8%(24/29), regardless of FR expression.
|
||||
| Experiment 9 Reporting the Activity Data of This PDC | [5] | ||||
| Indication | Ovarian clear cell carcinoma | ||||
| Efficacy Data | Disease control rate (DCR) | 62.50% | |||
| Patients Enrolled |
16 platinum-resistant ovarian clear cell carcinoma patients.
|
||||
| Administration Dosage | 0.15 mg/kg | ||||
| MOA of PDC |
Folate receptor α (FRα) and vanilloid subfamily member 6 of transient receptor potential channels (TRPV6) are potential promising therapeutic targets due to their high expression level in many solid tumors including ovarian cancer. CBP-1008 is a first-in-class (FIC) bi-specific ligand drug conjugate targeting FRα and TRPV6 carrying monomethyl auristatin E (MMAE) as payload.
Click to Show/Hide
|
||||
| Description |
OCCC accounts for 5% to 25% of OC1, and current treatment options have very poor ORR of <10%. The ORR of CBP-1008 (0.15 or 0.17 mg/kg) for OCCC patients was 31.3% (5/16), regardless of FR expression.
|
||||
| Experiment 10 Reporting the Activity Data of This PDC | [5] | ||||
| Indication | Ovarian cancer | ||||
| Efficacy Data | Disease control rate (DCR) | 82.80% | |||
| Patients Enrolled |
29 platinum-resistant ovarian cancer patients.
|
||||
| Administration Dosage | 0.15 mg/kg | ||||
| MOA of PDC |
Folate receptor α (FRα) and vanilloid subfamily member 6 of transient receptor potential channels (TRPV6) are potential promising therapeutic targets due to their high expression level in many solid tumors including ovarian cancer. CBP-1008 is a first-in-class (FIC) bi-specific ligand drug conjugate targeting FRα and TRPV6 carrying monomethyl auristatin E (MMAE) as payload.
Click to Show/Hide
|
||||
| Description |
Promising efficacy was observed in HGSOC patients (pts) who received prior 1-2L of TIT (if prior 2L, ≥12m of time interval between 2L; and ≥3m of time interval from the last TIT to CBP-1008 first dose). The ORR is 48.3%(14/29) and DCR is 82.8%(24/29), regardless of FR expression.
|
||||
BT5528 [Phase 1/2]
Discovered Using Cell Line-derived Xenograft Model
| Experiment 1 Reporting the Activity Data of This PDC | [7] | ||||
| Indication | Fibrosarcoma | ||||
| Efficacy Data | Tumor volume | 1200 mm3 | |||
| Administration Time | 20 day | ||||
| Administration Dosage | 0.167 mg/kg every week | ||||
| MOA of PDC |
Here we describe the development of BT5528, a bicyclic peptide (Bicycle) conjugated to the auristatin derivative maleimidocaproyl-monomethyl auristatin E to generate the Bicycle toxin conjugate BT5528. There are two potential mechanism of BT5528 bystander activity: extracellular linker cleavage and toxin penetration into neighboring cells, or receptor internalization and intracellular linker cleavage followed by release of cell penetrant toxin from lysed cells. The available data do not allow us to distinguish between these two mechanisms and it seems likely that BT5528 activity is mediated by toxin release following a combination of intracellular and extracellular linker cleavage.
Click to Show/Hide
|
||||
| Description |
BT5528 is efficacious in the PC3 xenograft model but control BTCs with noncleavable linkers and non-cell penetrant toxins lack comparable efficacy. A, The nonbinding BTC, BCY8245, is less active than BT5528 in the PC3 model (group mean ± SEM, n = 5) at both 0.5 and 0.0167 mg/kg dosing level (*, P < 0.05; **, P < 0.01; two-way ANOVA with Sidak's multiple comparisons test). B, Replacement of the cell penetrant toxin (MMAE: BT5528) with the non-cell penetrant toxin (MMAF: BCY10188) reduces activity in the PC3 model at 3, 1, and 0.33 mg/kg (group mean ± SEM; n = 5; *, P < 0.05; **, P < 0.01; two-way ANOVA with Sidak's multiple comparisons test). C, noncleavable linker chemistry abolishes activity in the HT1080 model; BCY6063, 10 mg/kg twice a week (group mean ± SEM, n = 3).
Click to Show/Hide
|
||||
| In Vivo Model | HT108 cells xenograft models in 6- to 8-week-old female balb/c nude or CB17-SCID mice. | ||||
| In Vitro Model | Fibrosarcoma | HT-1080 cell | CVCL_0317 | ||
| Half life period | 0.4 hour (Mouse); 0.3 hour (Rat); 0.6 hour (Nonhuman primate) | ||||
| Experiment 2 Reporting the Activity Data of This PDC | [7] | ||||
| Indication | Fibrosarcoma | ||||
| Efficacy Data | Tumor volume | 2200 mm3 | |||
| Administration Time | 20 day | ||||
| Administration Dosage | 0.5 mg/kg every week | ||||
| MOA of PDC |
Here we describe the development of BT5528, a bicyclic peptide (Bicycle) conjugated to the auristatin derivative maleimidocaproyl-monomethyl auristatin E to generate the Bicycle toxin conjugate BT5528. There are two potential mechanism of BT5528 bystander activity: extracellular linker cleavage and toxin penetration into neighboring cells, or receptor internalization and intracellular linker cleavage followed by release of cell penetrant toxin from lysed cells. The available data do not allow us to distinguish between these two mechanisms and it seems likely that BT5528 activity is mediated by toxin release following a combination of intracellular and extracellular linker cleavage.
Click to Show/Hide
|
||||
| Description |
BT5528 is efficacious in the PC3 xenograft model but control BTCs with noncleavable linkers and non-cell penetrant toxins lack comparable efficacy. A, The nonbinding BTC, BCY8245, is less active than BT5528 in the PC3 model (group mean ± SEM, n = 5) at both 0.5 and 0.0167 mg/kg dosing level (*, P < 0.05; **, P < 0.01; two-way ANOVA with Sidak's multiple comparisons test). B, Replacement of the cell penetrant toxin (MMAE: BT5528) with the non-cell penetrant toxin (MMAF: BCY10188) reduces activity in the PC3 model at 3, 1, and 0.33 mg/kg (group mean ± SEM; n = 5; *, P < 0.05; **, P < 0.01; two-way ANOVA with Sidak's multiple comparisons test). C, noncleavable linker chemistry abolishes activity in the HT1080 model; BCY6063, 10 mg/kg twice a week (group mean ± SEM, n = 3).
Click to Show/Hide
|
||||
| In Vivo Model | HT108 cells xenograft models in 6- to 8-week-old female balb/c nude or CB17-SCID mice. | ||||
| In Vitro Model | Fibrosarcoma | HT-1080 cell | CVCL_0317 | ||
| Half life period | 0.4 hour (Mouse); 0.3 hour (Rat); 0.6 hour (Nonhuman primate) | ||||
CBP-1018 [Phase 1]
Identified from the Human Clinical Data
| Experiment 1 Reporting the Activity Data of This PDC | [8] | ||||
| Indication | Solid tumor | ||||
| Efficacy Data | WBC decrease | 40% | |||
| Patients Enrolled |
20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma).
|
||||
| Administration Time | 4 week | ||||
| Administration Dosage | 0.03 mg/kg | ||||
| MOA of PDC |
Prostate-specific membrane antigen (PSMA) is highly expressed on prostate cancer and folate receptor α (FRα) overexpressed in various malignant tissues which both related to tumor invasiveness. CBP-1018 is a first-in-class bi-ligand-drug conjugate targeting both PSMA and FRα with monomethyl auristatin E (MMAE) as payload.
|
||||
| Description |
As of 27 April 2023, 20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma) were enrolled at 6 dose levels (DLs). No DLTs or drug-related deaths were observed. For 15 patients (75%) experienced treatment-related adverse events (TRAEs) ≥ grade 3, most common were neutrophil decrease (50%), WBC decrease (40%), hypokalemia (10%) and hypertriglyceridaemia (10%). Among 17 evaluable mCRPC patients, 5 SD and 7 Non-PD were observed with 9 patients delayed administration and 6 patients dropped for Covid-19. Prostate-specific antigen (PSA) 50% decrease was detected in 2 patients. The median PFS was 9.2 months (95%CI, 1.7-9.2) in mCRPC patients. For PK profile of CBP-1018 and free MMAE, t1/2z was ranged 0.54-1.15 h and 38.27-57.27 h, respectively, no accumulation of both substances after multiple doses.
Click to Show/Hide
|
||||
| Half life period | 0.54-1.15 h | ||||
| Experiment 2 Reporting the Activity Data of This PDC | [8] | ||||
| Indication | Solid tumor | ||||
| Efficacy Data | Stable disease (SD) | 29.40% | |||
| Patients Enrolled |
20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma).
|
||||
| Administration Time | 4 week | ||||
| Administration Dosage | 0.03 mg/kg | ||||
| MOA of PDC |
Prostate-specific membrane antigen (PSMA) is highly expressed on prostate cancer and folate receptor α (FRα) overexpressed in various malignant tissues which both related to tumor invasiveness. CBP-1018 is a first-in-class bi-ligand-drug conjugate targeting both PSMA and FRα with monomethyl auristatin E (MMAE) as payload.
|
||||
| Description |
As of 27 April 2023, 20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma) were enrolled at 6 dose levels (DLs). No DLTs or drug-related deaths were observed. For 15 patients (75%) experienced treatment-related adverse events (TRAEs) ≥ grade 3, most common were neutrophil decrease (50%), WBC decrease (40%), hypokalemia (10%) and hypertriglyceridaemia (10%). Among 17 evaluable mCRPC patients, 5 SD and 7 Non-PD were observed with 9 patients delayed administration and 6 patients dropped for Covid-19. Prostate-specific antigen (PSA) 50% decrease was detected in 2 patients. The median PFS was 9.2 months (95%CI, 1.7-9.2) in mCRPC patients. For PK profile of CBP-1018 and free MMAE, t1/2z was ranged 0.54-1.15 h and 38.27-57.27 h, respectively, no accumulation of both substances after multiple doses.
Click to Show/Hide
|
||||
| Half life period | 0.54-1.15 h | ||||
| Experiment 3 Reporting the Activity Data of This PDC | [8] | ||||
| Indication | Solid tumor | ||||
| Efficacy Data | Non-progressive disease (Non-PD) | 41.10% | |||
| Patients Enrolled |
20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma).
|
||||
| Administration Time | 4 week | ||||
| Administration Dosage | 0.03 mg/kg | ||||
| MOA of PDC |
Prostate-specific membrane antigen (PSMA) is highly expressed on prostate cancer and folate receptor α (FRα) overexpressed in various malignant tissues which both related to tumor invasiveness. CBP-1018 is a first-in-class bi-ligand-drug conjugate targeting both PSMA and FRα with monomethyl auristatin E (MMAE) as payload.
|
||||
| Description |
As of 27 April 2023, 20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma) were enrolled at 6 dose levels (DLs). No DLTs or drug-related deaths were observed. For 15 patients (75%) experienced treatment-related adverse events (TRAEs) ≥ grade 3, most common were neutrophil decrease (50%), WBC decrease (40%), hypokalemia (10%) and hypertriglyceridaemia (10%). Among 17 evaluable mCRPC patients, 5 SD and 7 Non-PD were observed with 9 patients delayed administration and 6 patients dropped for Covid-19. Prostate-specific antigen (PSA) 50% decrease was detected in 2 patients. The median PFS was 9.2 months (95%CI, 1.7-9.2) in mCRPC patients. For PK profile of CBP-1018 and free MMAE, t1/2z was ranged 0.54-1.15 h and 38.27-57.27 h, respectively, no accumulation of both substances after multiple doses.
Click to Show/Hide
|
||||
| Half life period | 0.54-1.15 h | ||||
| Experiment 4 Reporting the Activity Data of This PDC | [8] | ||||
| Indication | Solid tumor | ||||
| Efficacy Data | Neutrophil decrease | 50% | |||
| Patients Enrolled |
20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma).
|
||||
| Administration Time | 4 week | ||||
| Administration Dosage | 0.03 mg/kg | ||||
| MOA of PDC |
Prostate-specific membrane antigen (PSMA) is highly expressed on prostate cancer and folate receptor α (FRα) overexpressed in various malignant tissues which both related to tumor invasiveness. CBP-1018 is a first-in-class bi-ligand-drug conjugate targeting both PSMA and FRα with monomethyl auristatin E (MMAE) as payload.
|
||||
| Description |
As of 27 April 2023, 20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma) were enrolled at 6 dose levels (DLs). No DLTs or drug-related deaths were observed. For 15 patients (75%) experienced treatment-related adverse events (TRAEs) ≥ grade 3, most common were neutrophil decrease (50%), WBC decrease (40%), hypokalemia (10%) and hypertriglyceridaemia (10%). Among 17 evaluable mCRPC patients, 5 SD and 7 Non-PD were observed with 9 patients delayed administration and 6 patients dropped for Covid-19. Prostate-specific antigen (PSA) 50% decrease was detected in 2 patients. The median PFS was 9.2 months (95%CI, 1.7-9.2) in mCRPC patients. For PK profile of CBP-1018 and free MMAE, t1/2z was ranged 0.54-1.15 h and 38.27-57.27 h, respectively, no accumulation of both substances after multiple doses.
Click to Show/Hide
|
||||
| Half life period | 0.54-1.15 h | ||||
| Experiment 5 Reporting the Activity Data of This PDC | [8] | ||||
| Indication | Solid tumor | ||||
| Efficacy Data | Hypokalemia | 10% | |||
| Patients Enrolled |
20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma).
|
||||
| Administration Time | 4 week | ||||
| Administration Dosage | 0.03 mg/kg | ||||
| MOA of PDC |
Prostate-specific membrane antigen (PSMA) is highly expressed on prostate cancer and folate receptor α (FRα) overexpressed in various malignant tissues which both related to tumor invasiveness. CBP-1018 is a first-in-class bi-ligand-drug conjugate targeting both PSMA and FRα with monomethyl auristatin E (MMAE) as payload.
|
||||
| Description |
As of 27 April 2023, 20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma) were enrolled at 6 dose levels (DLs). No DLTs or drug-related deaths were observed. For 15 patients (75%) experienced treatment-related adverse events (TRAEs) ≥ grade 3, most common were neutrophil decrease (50%), WBC decrease (40%), hypokalemia (10%) and hypertriglyceridaemia (10%). Among 17 evaluable mCRPC patients, 5 SD and 7 Non-PD were observed with 9 patients delayed administration and 6 patients dropped for Covid-19. Prostate-specific antigen (PSA) 50% decrease was detected in 2 patients. The median PFS was 9.2 months (95%CI, 1.7-9.2) in mCRPC patients. For PK profile of CBP-1018 and free MMAE, t1/2z was ranged 0.54-1.15 h and 38.27-57.27 h, respectively, no accumulation of both substances after multiple doses.
Click to Show/Hide
|
||||
| Half life period | 0.54-1.15 h | ||||
| Experiment 6 Reporting the Activity Data of This PDC | [8] | ||||
| Indication | Solid tumor | ||||
| Efficacy Data | Hypertriglyceridaemia | 10% | |||
| Patients Enrolled |
20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma).
|
||||
| Administration Time | 4 week | ||||
| Administration Dosage | 0.03 mg/kg | ||||
| MOA of PDC |
Prostate-specific membrane antigen (PSMA) is highly expressed on prostate cancer and folate receptor α (FRα) overexpressed in various malignant tissues which both related to tumor invasiveness. CBP-1018 is a first-in-class bi-ligand-drug conjugate targeting both PSMA and FRα with monomethyl auristatin E (MMAE) as payload.
|
||||
| Description |
As of 27 April 2023, 20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma) were enrolled at 6 dose levels (DLs). No DLTs or drug-related deaths were observed. For 15 patients (75%) experienced treatment-related adverse events (TRAEs) ≥ grade 3, most common were neutrophil decrease (50%), WBC decrease (40%), hypokalemia (10%) and hypertriglyceridaemia (10%). Among 17 evaluable mCRPC patients, 5 SD and 7 Non-PD were observed with 9 patients delayed administration and 6 patients dropped for Covid-19. Prostate-specific antigen (PSA) 50% decrease was detected in 2 patients. The median PFS was 9.2 months (95%CI, 1.7-9.2) in mCRPC patients. For PK profile of CBP-1018 and free MMAE, t1/2z was ranged 0.54-1.15 h and 38.27-57.27 h, respectively, no accumulation of both substances after multiple doses.
Click to Show/Hide
|
||||
| Half life period | 0.54-1.15 h | ||||
| Experiment 7 Reporting the Activity Data of This PDC | [8] | ||||
| Indication | Solid tumor | ||||
| Efficacy Data | Grade ≥3 treatment-emergent adverse event rate | 75% | |||
| Patients Enrolled |
20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma).
|
||||
| Administration Time | 4 week | ||||
| Administration Dosage | 0.03 mg/kg | ||||
| MOA of PDC |
Prostate-specific membrane antigen (PSMA) is highly expressed on prostate cancer and folate receptor α (FRα) overexpressed in various malignant tissues which both related to tumor invasiveness. CBP-1018 is a first-in-class bi-ligand-drug conjugate targeting both PSMA and FRα with monomethyl auristatin E (MMAE) as payload.
|
||||
| Description |
As of 27 April 2023, 20 patients (18 mCRPC, 1 bladder cancer and 1 ureteral carcinoma) were enrolled at 6 dose levels (DLs). No DLTs or drug-related deaths were observed. For 15 patients (75%) experienced treatment-related adverse events (TRAEs) ≥ grade 3, most common were neutrophil decrease (50%), WBC decrease (40%), hypokalemia (10%) and hypertriglyceridaemia (10%). Among 17 evaluable mCRPC patients, 5 SD and 7 Non-PD were observed with 9 patients delayed administration and 6 patients dropped for Covid-19. Prostate-specific antigen (PSA) 50% decrease was detected in 2 patients. The median PFS was 9.2 months (95%CI, 1.7-9.2) in mCRPC patients. For PK profile of CBP-1018 and free MMAE, t1/2z was ranged 0.54-1.15 h and 38.27-57.27 h, respectively, no accumulation of both substances after multiple doses.
Click to Show/Hide
|
||||
| Half life period | 0.54-1.15 h | ||||
cyclo[DKP-isoDGR]-PEG4-GPLG-PABC-MMAE [Investigative]
Revealed Based on the Cell Line Data
| Experiment 1 Reporting the Activity Data of This PDC | [9] | ||||
| Indication | Ovarian serous cystadenocarcinoma | ||||
| Efficacy Data | Half maximal inhibitory concentration (IC50) | 3.7 ± 0.3 nM | |||
| Evaluation Method | MTT assay | ||||
| Administration Time | 72 h | ||||
| MOA of PDC |
Here, we show that the replacement of the Val-Ala-p-aminobenzyloxycarbamate linker with the Gly-Pro-Leu-Gly-p-aminobenzyloxycarbamate (GPLG-PABC) sequence as enzymatically cleavable linker in the SMDC bearing the cyclo[DKP-isoDGR] αVβ3 integrin ligand as tumor homing moiety and the monomethyl auristatin E (MMAE) as cytotoxic payload led to a 4-fold more potent anti-tumoral effect of the final conjugate on different cancer cell lines. In addition, the synthesized conjugate resulted to be significantly more potent than the free MMAE when tested following the kiss-and-run protocol, and the relative potency were clearly consistent with the expression of the αVβ3 integrin receptor in the considered cancer cell lines. In vitro enzymatic cleavage tests showed that the GPLG-PABC linker is cleaved by lysosomal enzymes, and that the released drug is observable already after 15 min of incubation. Although additional data are needed to fully characterize the releasing capacity of GPLG-PABC linker, our findings are of therapeutic significance since we are introducing an alternative to other well-established enzymatically sensitive peptide sequences that might be used in the future for generating more efficient and less toxic drug delivery systems.
Click to Show/Hide
|
||||
| Description |
In a first instance we performed an in vitro antiproliferative assay in which the different cell lines were incubated with different concentrations of the conjugate 2 for 72 h. As reported in Figure 3, 2 showed a potent antitumor activity in a low nanomolar range, from 3.7 to 70.4 nM depending on the cancer cell line, whereas the treatment with the free drug MMAE led to an antitumor activity of 0.03 nM for SK-OV-3 and of 0.23 nM for U87MG, and in very low nanomolar range on SK-MEL-28 cell line. Interestingly, the relative potency (RP) of the conjugate, normalized with respect to MMAE (i.e., the ratio of the IC50 values of 2 vs. MMAE) in U87MG cancer cell line after 72 h was much lower than the one observed with the previously reported cyclo[DKP-isoDGR]-PEG4-VA-PABC-MMAE (33-fold loss of potency vs. 151-fold loss of potency, respectively) bearing the VA linker. This data could suggest a positive effect of the GPLG cleavable linker on the release of the MMAE. Furthermore, a drop of potency between the free drug and the conjugate can be noticed in A549 from the RP value, where the integrin receptor level is significantly lower than in the other cancer cell lines. To better explore the targeting ability of the conjugate 2 towards different level of integrin expression, we decided to further evaluate the antiproliferative activity of the GPLG-conjugate by changing the incubation time.
Click to Show/Hide
|
||||
| In Vitro Model | Ovarian serous cystadenocarcinoma | SK-OV-3 cell | CVCL_0532 | ||
| Experiment 2 Reporting the Activity Data of This PDC | [9] | ||||
| Indication | Glioblastoma | ||||
| Efficacy Data | Half maximal inhibitory concentration (IC50) | 7.5 ± 0.9 nM | |||
| Evaluation Method | MTT assay | ||||
| Administration Time | 72 h | ||||
| MOA of PDC |
Here, we show that the replacement of the Val-Ala-p-aminobenzyloxycarbamate linker with the Gly-Pro-Leu-Gly-p-aminobenzyloxycarbamate (GPLG-PABC) sequence as enzymatically cleavable linker in the SMDC bearing the cyclo[DKP-isoDGR] αVβ3 integrin ligand as tumor homing moiety and the monomethyl auristatin E (MMAE) as cytotoxic payload led to a 4-fold more potent anti-tumoral effect of the final conjugate on different cancer cell lines. In addition, the synthesized conjugate resulted to be significantly more potent than the free MMAE when tested following the kiss-and-run protocol, and the relative potency were clearly consistent with the expression of the αVβ3 integrin receptor in the considered cancer cell lines. In vitro enzymatic cleavage tests showed that the GPLG-PABC linker is cleaved by lysosomal enzymes, and that the released drug is observable already after 15 min of incubation. Although additional data are needed to fully characterize the releasing capacity of GPLG-PABC linker, our findings are of therapeutic significance since we are introducing an alternative to other well-established enzymatically sensitive peptide sequences that might be used in the future for generating more efficient and less toxic drug delivery systems.
Click to Show/Hide
|
||||
| Description |
In a first instance we performed an in vitro antiproliferative assay in which the different cell lines were incubated with different concentrations of the conjugate 2 for 72 h. As reported in Figure 3, 2 showed a potent antitumor activity in a low nanomolar range, from 3.7 to 70.4 nM depending on the cancer cell line, whereas the treatment with the free drug MMAE led to an antitumor activity of 0.03 nM for SK-OV-3 and of 0.23 nM for U87MG, and in very low nanomolar range on SK-MEL-28 cell line. Interestingly, the relative potency (RP) of the conjugate, normalized with respect to MMAE (i.e., the ratio of the IC50 values of 2 vs. MMAE) in U87MG cancer cell line after 72 h was much lower than the one observed with the previously reported cyclo[DKP-isoDGR]-PEG4-VA-PABC-MMAE (33-fold loss of potency vs. 151-fold loss of potency, respectively) bearing the VA linker. This data could suggest a positive effect of the GPLG cleavable linker on the release of the MMAE. Furthermore, a drop of potency between the free drug and the conjugate can be noticed in A549 from the RP value, where the integrin receptor level is significantly lower than in the other cancer cell lines. To better explore the targeting ability of the conjugate 2 towards different level of integrin expression, we decided to further evaluate the antiproliferative activity of the GPLG-conjugate by changing the incubation time.
Click to Show/Hide
|
||||
| In Vitro Model | Glioblastoma | U-87MG cell | CVCL_0022 | ||
| Experiment 3 Reporting the Activity Data of This PDC | [9] | ||||
| Indication | Lung adenocarcinoma | ||||
| Efficacy Data | Half maximal inhibitory concentration (IC50) | 20.8 ± 1.8 nM | |||
| Evaluation Method | MTT assay | ||||
| Administration Time | 72 h | ||||
| MOA of PDC |
Here, we show that the replacement of the Val-Ala-p-aminobenzyloxycarbamate linker with the Gly-Pro-Leu-Gly-p-aminobenzyloxycarbamate (GPLG-PABC) sequence as enzymatically cleavable linker in the SMDC bearing the cyclo[DKP-isoDGR] αVβ3 integrin ligand as tumor homing moiety and the monomethyl auristatin E (MMAE) as cytotoxic payload led to a 4-fold more potent anti-tumoral effect of the final conjugate on different cancer cell lines. In addition, the synthesized conjugate resulted to be significantly more potent than the free MMAE when tested following the kiss-and-run protocol, and the relative potency were clearly consistent with the expression of the αVβ3 integrin receptor in the considered cancer cell lines. In vitro enzymatic cleavage tests showed that the GPLG-PABC linker is cleaved by lysosomal enzymes, and that the released drug is observable already after 15 min of incubation. Although additional data are needed to fully characterize the releasing capacity of GPLG-PABC linker, our findings are of therapeutic significance since we are introducing an alternative to other well-established enzymatically sensitive peptide sequences that might be used in the future for generating more efficient and less toxic drug delivery systems.
Click to Show/Hide
|
||||
| Description |
In a first instance we performed an in vitro antiproliferative assay in which the different cell lines were incubated with different concentrations of the conjugate 2 for 72 h. As reported in Figure 3, 2 showed a potent antitumor activity in a low nanomolar range, from 3.7 to 70.4 nM depending on the cancer cell line, whereas the treatment with the free drug MMAE led to an antitumor activity of 0.03 nM for SK-OV-3 and of 0.23 nM for U87MG, and in very low nanomolar range on SK-MEL-28 cell line. Interestingly, the relative potency (RP) of the conjugate, normalized with respect to MMAE (i.e., the ratio of the IC50 values of 2 vs. MMAE) in U87MG cancer cell line after 72 h was much lower than the one observed with the previously reported cyclo[DKP-isoDGR]-PEG4-VA-PABC-MMAE (33-fold loss of potency vs. 151-fold loss of potency, respectively) bearing the VA linker. This data could suggest a positive effect of the GPLG cleavable linker on the release of the MMAE. Furthermore, a drop of potency between the free drug and the conjugate can be noticed in A549 from the RP value, where the integrin receptor level is significantly lower than in the other cancer cell lines. To better explore the targeting ability of the conjugate 2 towards different level of integrin expression, we decided to further evaluate the antiproliferative activity of the GPLG-conjugate by changing the incubation time.
Click to Show/Hide
|
||||
| In Vitro Model | Lung adenocarcinoma | A-549 cell | CVCL_0023 | ||
| Experiment 4 Reporting the Activity Data of This PDC | [9] | ||||
| Indication | Melanoma | ||||
| Efficacy Data | Half maximal inhibitory concentration (IC50) | 70.4 ± 7.1 nM | |||
| Evaluation Method | MTT assay | ||||
| Administration Time | 72 h | ||||
| MOA of PDC |
Here, we show that the replacement of the Val-Ala-p-aminobenzyloxycarbamate linker with the Gly-Pro-Leu-Gly-p-aminobenzyloxycarbamate (GPLG-PABC) sequence as enzymatically cleavable linker in the SMDC bearing the cyclo[DKP-isoDGR] αVβ3 integrin ligand as tumor homing moiety and the monomethyl auristatin E (MMAE) as cytotoxic payload led to a 4-fold more potent anti-tumoral effect of the final conjugate on different cancer cell lines. In addition, the synthesized conjugate resulted to be significantly more potent than the free MMAE when tested following the kiss-and-run protocol, and the relative potency were clearly consistent with the expression of the αVβ3 integrin receptor in the considered cancer cell lines. In vitro enzymatic cleavage tests showed that the GPLG-PABC linker is cleaved by lysosomal enzymes, and that the released drug is observable already after 15 min of incubation. Although additional data are needed to fully characterize the releasing capacity of GPLG-PABC linker, our findings are of therapeutic significance since we are introducing an alternative to other well-established enzymatically sensitive peptide sequences that might be used in the future for generating more efficient and less toxic drug delivery systems.
Click to Show/Hide
|
||||
| Description |
In a first instance we performed an in vitro antiproliferative assay in which the different cell lines were incubated with different concentrations of the conjugate 2 for 72 h. As reported in Figure 3, 2 showed a potent antitumor activity in a low nanomolar range, from 3.7 to 70.4 nM depending on the cancer cell line, whereas the treatment with the free drug MMAE led to an antitumor activity of 0.03 nM for SK-OV-3 and of 0.23 nM for U87MG, and in very low nanomolar range on SK-MEL-28 cell line. Interestingly, the relative potency (RP) of the conjugate, normalized with respect to MMAE (i.e., the ratio of the IC50 values of 2 vs. MMAE) in U87MG cancer cell line after 72 h was much lower than the one observed with the previously reported cyclo[DKP-isoDGR]-PEG4-VA-PABC-MMAE (33-fold loss of potency vs. 151-fold loss of potency, respectively) bearing the VA linker. This data could suggest a positive effect of the GPLG cleavable linker on the release of the MMAE. Furthermore, a drop of potency between the free drug and the conjugate can be noticed in A549 from the RP value, where the integrin receptor level is significantly lower than in the other cancer cell lines. To better explore the targeting ability of the conjugate 2 towards different level of integrin expression, we decided to further evaluate the antiproliferative activity of the GPLG-conjugate by changing the incubation time.
Click to Show/Hide
|
||||
| In Vitro Model | Melanoma | SK-MEL-202 cell | CVCL_6106 | ||
1131-MMAE [Investigative]
Revealed Based on the Cell Line Data
| Experiment 1 Reporting the Activity Data of This PDC | [3] | ||||
| Indication | Gastric cancer | ||||
| Efficacy Data | Half Maximal Inhibitory Concentration (IC50) | 3.87 nM | |||
| Administration Time | 72 h | ||||
| Description |
We next evaluated the in vitro cytotoxicity of 1131-MMAE. NUGC-4, MKN45 and HGC27 cells were drug-treated for 72 h and their viability was assessed. 1131-MMAE killed KK-LC-1 positive gastric cancer cells with high potency. The IC50 values of 1131-MMAE were 3.87 nM for NUGC-4 cells and 5.26 nM for MKN45 cells. However, although a very high concentration was used, 1131-MMAE could only moderately inhibit the viability of KK-LC-1 negative HGC27 cells. The IC50 value of 1131-MMAE for HGC27 cells was 100-200 times higher than that in NUGC-4 and MNK45 cells. Free MMAE exerted cytotoxicity irrespective of the KK-LC-1 expression status. The IC50 values of free MMAE were 10.97 nM for NUGC-4 cells, 10.70 nM for MKN45 cells and 7.18 nM for HGC27 cells. Naked 1131 peptide showed no cytotoxicity to all three cell lines. These results were consistent with the KK-LC-1-dependent endocytosis and confirmed the target-selective killing of 1131-MMAE.
Click to Show/Hide
|
||||
| In Vitro Model | Gastric signet ring cell adenocarcinoma | NUGC-4 cell | CVCL_3082 | ||
| Experiment 2 Reporting the Activity Data of This PDC | [3] | ||||
| Indication | Gastric cancer | ||||
| Efficacy Data | Half Maximal Inhibitory Concentration (IC50) | 5.26 nM | |||
| Administration Time | 72 h | ||||
| Description |
We next evaluated the in vitro cytotoxicity of 1131-MMAE. NUGC-4, MKN45 and HGC27 cells were drug-treated for 72 h and their viability was assessed. 1131-MMAE killed KK-LC-1 positive gastric cancer cells with high potency. The IC50 values of 1131-MMAE were 3.87 nM for NUGC-4 cells and 5.26 nM for MKN45 cells. However, although a very high concentration was used, 1131-MMAE could only moderately inhibit the viability of KK-LC-1 negative HGC27 cells. The IC50 value of 1131-MMAE for HGC27 cells was 100-200 times higher than that in NUGC-4 and MNK45 cells. Free MMAE exerted cytotoxicity irrespective of the KK-LC-1 expression status. The IC50 values of free MMAE were 10.97 nM for NUGC-4 cells, 10.70 nM for MKN45 cells and 7.18 nM for HGC27 cells. Naked 1131 peptide showed no cytotoxicity to all three cell lines. These results were consistent with the KK-LC-1-dependent endocytosis and confirmed the target-selective killing of 1131-MMAE.
Click to Show/Hide
|
||||
| In Vitro Model | Gastric adenocarcinoma | MKN45 cell | CVCL_0434 | ||
| Experiment 3 Reporting the Activity Data of This PDC | [3] | ||||
| Indication | Gastric cancer | ||||
| Efficacy Data | Half Maximal Inhibitory Concentration (IC50) | 786 nM | |||
| Administration Time | 72 h | ||||
| Description |
We next evaluated the in vitro cytotoxicity of 1131-MMAE. NUGC-4, MKN45 and HGC27 cells were drug-treated for 72 h and their viability was assessed. 1131-MMAE killed KK-LC-1 positive gastric cancer cells with high potency. The IC50 values of 1131-MMAE were 3.87 nM for NUGC-4 cells and 5.26 nM for MKN45 cells. However, although a very high concentration was used, 1131-MMAE could only moderately inhibit the viability of KK-LC-1 negative HGC27 cells. The IC50 value of 1131-MMAE for HGC27 cells was 100-200 times higher than that in NUGC-4 and MNK45 cells. Free MMAE exerted cytotoxicity irrespective of the KK-LC-1 expression status. The IC50 values of free MMAE were 10.97 nM for NUGC-4 cells, 10.70 nM for MKN45 cells and 7.18 nM for HGC27 cells. Naked 1131 peptide showed no cytotoxicity to all three cell lines. These results were consistent with the KK-LC-1-dependent endocytosis and confirmed the target-selective killing of 1131-MMAE.
Click to Show/Hide
|
||||
| In Vitro Model | Gastric carcinoma | HGC-27 cell | CVCL_1279 | ||
D-Cys6-LHRH vedotin [Investigative]
Revealed Based on the Cell Line Data
| Experiment 1 Reporting the Activity Data of This PDC | [2] | ||||
| Indication | Ovarian cancer | ||||
| Efficacy Data | Half Maximal growth inhibition concentration (GI50) | 4 nM | |||
| Administration Time | 3 days | ||||
| MOA of PDC |
Ovarian cancer is the most deadly female gynaecological malignancy in developed countries and new treatments are urgently needed. The luteinising hormone releasing hormone (LHRH) peptide drug conjugate Zoptarelin doxorubicin is one such potential new drug modality that entered clinical trials for treating LHRH receptor-positive gynaecological cancers. However, development stopped after disappointing Phase 3 results in 2017. We believe the lack of efficacy was due to linker instability and payload potency. In this work, we replaced its linker-toxin with vedotin (MC-VC-PABC-MMAE), yielding the novel peptide drug conjugate D-Cys6-LHRH vedotin. A GI50 and cell specificity comparison against cancerous and non-cancerous ovarian cell lines showed significantly superior bioactivity and selectivity over Zoptarelin doxorubicin (GI50 4 vs. 453 nM) and other chemotherapeutic drugs used for treating ovarian cancers. Our results suggest D-Cys6-LHRH vedotin can potentially be used as a treatment for ovarian cancer.
Click to Show/Hide
|
||||
| Description |
GI50s are summarised in Table 1. Our cell panel consisted of LHRH receptor-positive (OVCAR-3) and receptor-negative (SK-OV-3) ovarian cancer cell lines used in Zoptarelin doxorubicin's preclinical development studies. Non-cancerous human ovarian (H-6036) and lung fibroblast (MRC-5) cell lines were also included for selectivity comparison. Paclitaxel, a first-line chemotherapeutic drug used for ovarian cancer, was observed to be highly cytotoxic against all cell lines, including non-cancerous ovarian and human fibroblasts (GI50s 1-5 nM). Unsurprisingly, common and serious side-effects experienced by more than 50% patients dosed with this drug included anaemia, neutropenia, peripheral neuropathy, nausea, vomiting, myalgia, arthralgia and alopecia. Similarly, doxorubicin was also shown to be non-specific towards all the cell lines (GI50s 60-311 nM), below the reported average 631 nM GI50 in a study involving 39 cancer cell lines. It is noteworthy that doxorubicin exhibited moderate GI50s of 311 and 218 nM against OVCAR-3 and SK-OV-3, respectively, supporting earlier in vitro data. Tubulin binder MMAE was found to be ultra-toxic against all cell lines (GI50s 0.5-1.1 nM), supporting the findings from an earlier report. It is therefore unsurprising that MMAE has never been approved as a drug on its own. The LHRH analog and carrier peptide, D-Cys6-LHRH, was inactive against all cell lines (GI50s >50,000 nM).
Click to Show/Hide
|
||||
| In Vitro Model | Ovarian serous adenocarcinoma | OVCAR-3 cell | CVCL_0465 | ||
| Experiment 2 Reporting the Activity Data of This PDC | [2] | ||||
| Indication | Ovarian cancer | ||||
| Efficacy Data | Half Maximal growth inhibition concentration (GI50) | 49 nM | |||
| Administration Time | 3 days | ||||
| MOA of PDC |
Ovarian cancer is the most deadly female gynaecological malignancy in developed countries and new treatments are urgently needed. The luteinising hormone releasing hormone (LHRH) peptide drug conjugate Zoptarelin doxorubicin is one such potential new drug modality that entered clinical trials for treating LHRH receptor-positive gynaecological cancers. However, development stopped after disappointing Phase 3 results in 2017. We believe the lack of efficacy was due to linker instability and payload potency. In this work, we replaced its linker-toxin with vedotin (MC-VC-PABC-MMAE), yielding the novel peptide drug conjugate D-Cys6-LHRH vedotin. A GI50 and cell specificity comparison against cancerous and non-cancerous ovarian cell lines showed significantly superior bioactivity and selectivity over Zoptarelin doxorubicin (GI50 4 vs. 453 nM) and other chemotherapeutic drugs used for treating ovarian cancers. Our results suggest D-Cys6-LHRH vedotin can potentially be used as a treatment for ovarian cancer.
Click to Show/Hide
|
||||
| Description |
GI50s are summarised in Table 1. Our cell panel consisted of LHRH receptor-positive (OVCAR-3) and receptor-negative (SK-OV-3) ovarian cancer cell lines used in Zoptarelin doxorubicin's preclinical development studies. Non-cancerous human ovarian (H-6036) and lung fibroblast (MRC-5) cell lines were also included for selectivity comparison. Paclitaxel, a first-line chemotherapeutic drug used for ovarian cancer, was observed to be highly cytotoxic against all cell lines, including non-cancerous ovarian and human fibroblasts (GI50s 1-5 nM). Unsurprisingly, common and serious side-effects experienced by more than 50% patients dosed with this drug included anaemia, neutropenia, peripheral neuropathy, nausea, vomiting, myalgia, arthralgia and alopecia. Similarly, doxorubicin was also shown to be non-specific towards all the cell lines (GI50s 60-311 nM), below the reported average 631 nM GI50 in a study involving 39 cancer cell lines. It is noteworthy that doxorubicin exhibited moderate GI50s of 311 and 218 nM against OVCAR-3 and SK-OV-3, respectively, supporting earlier in vitro data. Tubulin binder MMAE was found to be ultra-toxic against all cell lines (GI50s 0.5-1.1 nM), supporting the findings from an earlier report. It is therefore unsurprising that MMAE has never been approved as a drug on its own. The LHRH analog and carrier peptide, D-Cys6-LHRH, was inactive against all cell lines (GI50s >50,000 nM).
Click to Show/Hide
|
||||
| In Vitro Model | Ovarian serous cystadenocarcinoma | SK-OV-3 cell | CVCL_0532 | ||
| Experiment 3 Reporting the Activity Data of This PDC | [2] | ||||
| Indication | Ovarian cancer | ||||
| Efficacy Data | Half Maximal growth inhibition concentration (GI50) | 52 nM | |||
| Administration Time | 3 days | ||||
| MOA of PDC |
Ovarian cancer is the most deadly female gynaecological malignancy in developed countries and new treatments are urgently needed. The luteinising hormone releasing hormone (LHRH) peptide drug conjugate Zoptarelin doxorubicin is one such potential new drug modality that entered clinical trials for treating LHRH receptor-positive gynaecological cancers. However, development stopped after disappointing Phase 3 results in 2017. We believe the lack of efficacy was due to linker instability and payload potency. In this work, we replaced its linker-toxin with vedotin (MC-VC-PABC-MMAE), yielding the novel peptide drug conjugate D-Cys6-LHRH vedotin. A GI50 and cell specificity comparison against cancerous and non-cancerous ovarian cell lines showed significantly superior bioactivity and selectivity over Zoptarelin doxorubicin (GI50 4 vs. 453 nM) and other chemotherapeutic drugs used for treating ovarian cancers. Our results suggest D-Cys6-LHRH vedotin can potentially be used as a treatment for ovarian cancer.
Click to Show/Hide
|
||||
| Description |
GI50s are summarised in Table 1. Our cell panel consisted of LHRH receptor-positive (OVCAR-3) and receptor-negative (SK-OV-3) ovarian cancer cell lines used in Zoptarelin doxorubicin's preclinical development studies. Non-cancerous human ovarian (H-6036) and lung fibroblast (MRC-5) cell lines were also included for selectivity comparison. Paclitaxel, a first-line chemotherapeutic drug used for ovarian cancer, was observed to be highly cytotoxic against all cell lines, including non-cancerous ovarian and human fibroblasts (GI50s 1-5 nM). Unsurprisingly, common and serious side-effects experienced by more than 50% patients dosed with this drug included anaemia, neutropenia, peripheral neuropathy, nausea, vomiting, myalgia, arthralgia and alopecia. Similarly, doxorubicin was also shown to be non-specific towards all the cell lines (GI50s 60-311 nM), below the reported average 631 nM GI50 in a study involving 39 cancer cell lines. It is noteworthy that doxorubicin exhibited moderate GI50s of 311 and 218 nM against OVCAR-3 and SK-OV-3, respectively, supporting earlier in vitro data. Tubulin binder MMAE was found to be ultra-toxic against all cell lines (GI50s 0.5-1.1 nM), supporting the findings from an earlier report. It is therefore unsurprising that MMAE has never been approved as a drug on its own. The LHRH analog and carrier peptide, D-Cys6-LHRH, was inactive against all cell lines (GI50s >50,000 nM).
Click to Show/Hide
|
||||
| In Vitro Model | Normal | H-6036 cell | Homo sapiens | ||
| Experiment 4 Reporting the Activity Data of This PDC | [2] | ||||
| Indication | Ovarian cancer | ||||
| Efficacy Data | Half Maximal growth inhibition concentration (GI50) | 191 nM | |||
| Administration Time | 3 days | ||||
| MOA of PDC |
Ovarian cancer is the most deadly female gynaecological malignancy in developed countries and new treatments are urgently needed. The luteinising hormone releasing hormone (LHRH) peptide drug conjugate Zoptarelin doxorubicin is one such potential new drug modality that entered clinical trials for treating LHRH receptor-positive gynaecological cancers. However, development stopped after disappointing Phase 3 results in 2017. We believe the lack of efficacy was due to linker instability and payload potency. In this work, we replaced its linker-toxin with vedotin (MC-VC-PABC-MMAE), yielding the novel peptide drug conjugate D-Cys6-LHRH vedotin. A GI50 and cell specificity comparison against cancerous and non-cancerous ovarian cell lines showed significantly superior bioactivity and selectivity over Zoptarelin doxorubicin (GI50 4 vs. 453 nM) and other chemotherapeutic drugs used for treating ovarian cancers. Our results suggest D-Cys6-LHRH vedotin can potentially be used as a treatment for ovarian cancer.
Click to Show/Hide
|
||||
| Description |
GI50s are summarised in Table 1. Our cell panel consisted of LHRH receptor-positive (OVCAR-3) and receptor-negative (SK-OV-3) ovarian cancer cell lines used in Zoptarelin doxorubicin's preclinical development studies. Non-cancerous human ovarian (H-6036) and lung fibroblast (MRC-5) cell lines were also included for selectivity comparison. Paclitaxel, a first-line chemotherapeutic drug used for ovarian cancer, was observed to be highly cytotoxic against all cell lines, including non-cancerous ovarian and human fibroblasts (GI50s 1-5 nM). Unsurprisingly, common and serious side-effects experienced by more than 50% patients dosed with this drug included anaemia, neutropenia, peripheral neuropathy, nausea, vomiting, myalgia, arthralgia and alopecia. Similarly, doxorubicin was also shown to be non-specific towards all the cell lines (GI50s 60-311 nM), below the reported average 631 nM GI50 in a study involving 39 cancer cell lines. It is noteworthy that doxorubicin exhibited moderate GI50s of 311 and 218 nM against OVCAR-3 and SK-OV-3, respectively, supporting earlier in vitro data. Tubulin binder MMAE was found to be ultra-toxic against all cell lines (GI50s 0.5-1.1 nM), supporting the findings from an earlier report. It is therefore unsurprising that MMAE has never been approved as a drug on its own. The LHRH analog and carrier peptide, D-Cys6-LHRH, was inactive against all cell lines (GI50s >50,000 nM).
Click to Show/Hide
|
||||
| In Vitro Model | Normal | MRC-5 cell | CVCL_0440 | ||
[64Cu]PDC-1 [Investigative]
Revealed Based on the Cell Line Data
| Experiment 1 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Melanoma | ||||
| Efficacy Data | Half Maximal Effective Concentration (EC50) | 0.058 ± 0.003 nM | |||
| Evaluation Method | WST-1 assay | ||||
| Administration Time | 48 h | ||||
| MOA of PDC |
Many anticancer drugs exhibit high systemic off-target toxicities causing severe side effects. Peptide-drug conjugates (PDCs) that target tumor-specific receptors such as integrin vβ6 are emerging as powerful tools to overcome these challenges. The development of an integrin vβ6-selective PDC was achieved by combining the therapeutic efficacy of the cytotoxic drug monomethyl auristatin E with the selectivity of the vβ6-binding peptide (vβ6-BP) and with the ability of positron emission tomography (PET) imaging by copper-64. The [64Cu]PDC-1 was produced efficiently and in high purity. The PDC exhibited high human serum stability, integrin vβ6-selective internalization, cell binding, and cytotoxicity. Integrin vβ6-selective tumor accumulation of the [64Cu]PDC-1 was visualized with PET-imaging and corroborated by biodistribution, and [64Cu]PDC-1 showed promising in vivo pharmacokinetics. The [natCu]PDC-1 treatment resulted in prolonged survival of mice bearing vβ6 (+) tumors (median survival: 77 days, vs vβ6 (-) tumor group 49 days, and all other control groups 37 days).
Click to Show/Hide
|
||||
| Description |
Both NH2-PDC-1 and [natCu]PDC-1 exhibited integrin v6-dependent cytotoxicity, only reducing cell viability of the v6-positive cells. For [natCu]PDC-1 high cytotoxicity was observed in DX3puro6 (+) cells (EC50: 0.058 ± 0.003 nM) with no observable cytotoxic effects in the DX3puro (-) cells, while free MMAE had almost equal cytotoxicity to both DX3puro6 (+) and DX3puro cells (-) (EC50: 0.14-0.15 nM). The pancreatic cells also showed v6-dependent cytotoxicity for [natCu]PDC-1 (EC50: BxPC-3 65.1 ± 10.6 nM) and required high concentrations of ≥250 nM for noticeable cytotoxic effects in the minimally integrin v6-expressing MIA PaCa-2 cells. Again, free, non-targeted MMAE exhibited nondiscriminatory cytotoxicity among the pancreatic cells with an effective concentration range of EC50 = 0.16-0.5 nM. Peptides NH2-2 and [natCu]2 were not toxic to any cells.
Click to Show/Hide
|
||||
| In Vitro Model | Melanoma | DX3-puro/beta6 cell | CVCL_1D33 | ||
| Experiment 2 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Melanoma | ||||
| Efficacy Data | Half Maximal Effective Concentration (EC50) | > 5 nM | |||
| Evaluation Method | WST-1 assay | ||||
| Administration Time | 48 h | ||||
| MOA of PDC |
Many anticancer drugs exhibit high systemic off-target toxicities causing severe side effects. Peptide-drug conjugates (PDCs) that target tumor-specific receptors such as integrin vβ6 are emerging as powerful tools to overcome these challenges. The development of an integrin vβ6-selective PDC was achieved by combining the therapeutic efficacy of the cytotoxic drug monomethyl auristatin E with the selectivity of the vβ6-binding peptide (vβ6-BP) and with the ability of positron emission tomography (PET) imaging by copper-64. The [64Cu]PDC-1 was produced efficiently and in high purity. The PDC exhibited high human serum stability, integrin vβ6-selective internalization, cell binding, and cytotoxicity. Integrin vβ6-selective tumor accumulation of the [64Cu]PDC-1 was visualized with PET-imaging and corroborated by biodistribution, and [64Cu]PDC-1 showed promising in vivo pharmacokinetics. The [natCu]PDC-1 treatment resulted in prolonged survival of mice bearing vβ6 (+) tumors (median survival: 77 days, vs vβ6 (-) tumor group 49 days, and all other control groups 37 days).
Click to Show/Hide
|
||||
| Description |
Both NH2-PDC-1 and [natCu]PDC-1 exhibited integrin v6-dependent cytotoxicity, only reducing cell viability of the v6-positive cells. For [natCu]PDC-1 high cytotoxicity was observed in DX3puro6 (+) cells (EC50: 0.058 ± 0.003 nM) with no observable cytotoxic effects in the DX3puro (-) cells, while free MMAE had almost equal cytotoxicity to both DX3puro6 (+) and DX3puro cells (-) (EC50: 0.14-0.15 nM). The pancreatic cells also showed v6-dependent cytotoxicity for [natCu]PDC-1 (EC50: BxPC-3 65.1 ± 10.6 nM) and required high concentrations of ≥250 nM for noticeable cytotoxic effects in the minimally integrin v6-expressing MIA PaCa-2 cells. Again, free, non-targeted MMAE exhibited nondiscriminatory cytotoxicity among the pancreatic cells with an effective concentration range of EC50 = 0.16-0.5 nM. Peptides NH2-2 and [natCu]2 were not toxic to any cells.
Click to Show/Hide
|
||||
| In Vitro Model | Melanoma | DX3-puro cell | CVCL_1D33 | ||
| Experiment 3 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Pancreatic cancer | ||||
| Efficacy Data | Half Maximal Effective Concentration (EC50) | 65.1 ± 10.6 nM | |||
| Evaluation Method | WST-1 assay | ||||
| Administration Time | 48 h | ||||
| MOA of PDC |
Many anticancer drugs exhibit high systemic off-target toxicities causing severe side effects. Peptide-drug conjugates (PDCs) that target tumor-specific receptors such as integrin vβ6 are emerging as powerful tools to overcome these challenges. The development of an integrin vβ6-selective PDC was achieved by combining the therapeutic efficacy of the cytotoxic drug monomethyl auristatin E with the selectivity of the vβ6-binding peptide (vβ6-BP) and with the ability of positron emission tomography (PET) imaging by copper-64. The [64Cu]PDC-1 was produced efficiently and in high purity. The PDC exhibited high human serum stability, integrin vβ6-selective internalization, cell binding, and cytotoxicity. Integrin vβ6-selective tumor accumulation of the [64Cu]PDC-1 was visualized with PET-imaging and corroborated by biodistribution, and [64Cu]PDC-1 showed promising in vivo pharmacokinetics. The [natCu]PDC-1 treatment resulted in prolonged survival of mice bearing vβ6 (+) tumors (median survival: 77 days, vs vβ6 (-) tumor group 49 days, and all other control groups 37 days).
Click to Show/Hide
|
||||
| Description |
Both NH2-PDC-1 and [natCu]PDC-1 exhibited integrin v6-dependent cytotoxicity, only reducing cell viability of the v6-positive cells. For [natCu]PDC-1 high cytotoxicity was observed in DX3puro6 (+) cells (EC50: 0.058 ± 0.003 nM) with no observable cytotoxic effects in the DX3puro (-) cells, while free MMAE had almost equal cytotoxicity to both DX3puro6 (+) and DX3puro cells (-) (EC50: 0.14-0.15 nM). The pancreatic cells also showed v6-dependent cytotoxicity for [natCu]PDC-1 (EC50: BxPC-3 65.1 ± 10.6 nM) and required high concentrations of ≥250 nM for noticeable cytotoxic effects in the minimally integrin v6-expressing MIA PaCa-2 cells. Again, free, non-targeted MMAE exhibited nondiscriminatory cytotoxicity among the pancreatic cells with an effective concentration range of EC50 = 0.16-0.5 nM. Peptides NH2-2 and [natCu]2 were not toxic to any cells.
Click to Show/Hide
|
||||
| In Vitro Model | Pancreatic ductal adenocarcinoma | BxPC-3 (+) cells | CVCL_0186 | ||
| Experiment 4 Reporting the Activity Data of This PDC | [1] | ||||
| Indication | Pancreatic cancer | ||||
| Efficacy Data | Half Maximal Effective Concentration (EC50) | > 250 nM | |||
| Evaluation Method | WST-1 assay | ||||
| Administration Time | 48 h | ||||
| MOA of PDC |
Many anticancer drugs exhibit high systemic off-target toxicities causing severe side effects. Peptide-drug conjugates (PDCs) that target tumor-specific receptors such as integrin vβ6 are emerging as powerful tools to overcome these challenges. The development of an integrin vβ6-selective PDC was achieved by combining the therapeutic efficacy of the cytotoxic drug monomethyl auristatin E with the selectivity of the vβ6-binding peptide (vβ6-BP) and with the ability of positron emission tomography (PET) imaging by copper-64. The [64Cu]PDC-1 was produced efficiently and in high purity. The PDC exhibited high human serum stability, integrin vβ6-selective internalization, cell binding, and cytotoxicity. Integrin vβ6-selective tumor accumulation of the [64Cu]PDC-1 was visualized with PET-imaging and corroborated by biodistribution, and [64Cu]PDC-1 showed promising in vivo pharmacokinetics. The [natCu]PDC-1 treatment resulted in prolonged survival of mice bearing vβ6 (+) tumors (median survival: 77 days, vs vβ6 (-) tumor group 49 days, and all other control groups 37 days).
Click to Show/Hide
|
||||
| Description |
Both NH2-PDC-1 and [natCu]PDC-1 exhibited integrin v6-dependent cytotoxicity, only reducing cell viability of the v6-positive cells. For [natCu]PDC-1 high cytotoxicity was observed in DX3puro6 (+) cells (EC50: 0.058 ± 0.003 nM) with no observable cytotoxic effects in the DX3puro (-) cells, while free MMAE had almost equal cytotoxicity to both DX3puro6 (+) and DX3puro cells (-) (EC50: 0.14-0.15 nM). The pancreatic cells also showed v6-dependent cytotoxicity for [natCu]PDC-1 (EC50: BxPC-3 65.1 ± 10.6 nM) and required high concentrations of ≥250 nM for noticeable cytotoxic effects in the minimally integrin v6-expressing MIA PaCa-2 cells. Again, free, non-targeted MMAE exhibited nondiscriminatory cytotoxicity among the pancreatic cells with an effective concentration range of EC50 = 0.16-0.5 nM. Peptides NH2-2 and [natCu]2 were not toxic to any cells.
Click to Show/Hide
|
||||
| In Vitro Model | Pancreatic ductal adenocarcinoma | MIA PaCa-2 cell | CVCL_0428 | ||
References
